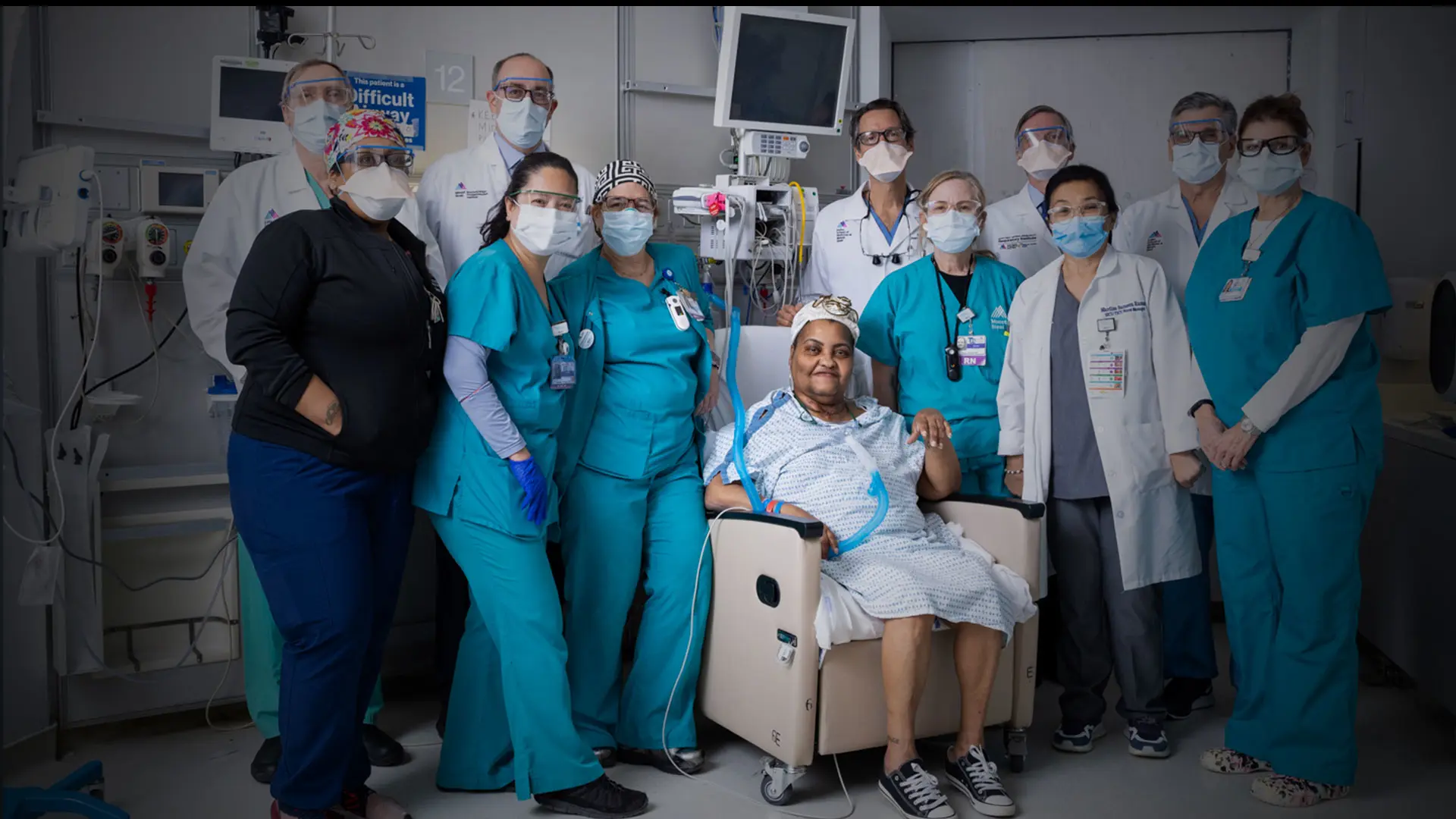
Through all of human history, thousands of people with long-segment tracheal defects died each year. Now, they have the opportunity to benefit from a life-saving new treatment.
With the emergence of COVID-19, the need for tracheal transplantation has become more critical. More than a year into the pandemic, there has been a stark rise in the number of patients with severe intubation damage from the prolonged use of ventilators.
In addition to patients with tracheal damage, future recipients may include those born with tracheal defects or individuals who have untreatable airway diseases, burns, or tumors.
The patient chosen to undergo this novel surgery is Sonia Sein a 56-year-old New Yorker who suffered tracheal damage after being intubated due to an asthma attack. Ms. Sein, who is a trained social worker, developed an 8 cm long-segment cricotracheal stenosis and, for the past six years, has lived in constant fear that she would go to sleep at night and never wake up. Now, she has a well-functioning trachea and has not experienced any complications or signs of organ rejection. She can breathe on her own and is no longer at risk of suffocation from progressive airway disease.
“Knowing that this procedure and 30 years of research will save countless lives was indescribable,” says Eric M. Genden, MD, MHCA, FACS. “It is why we do what we do: to make a difference.”
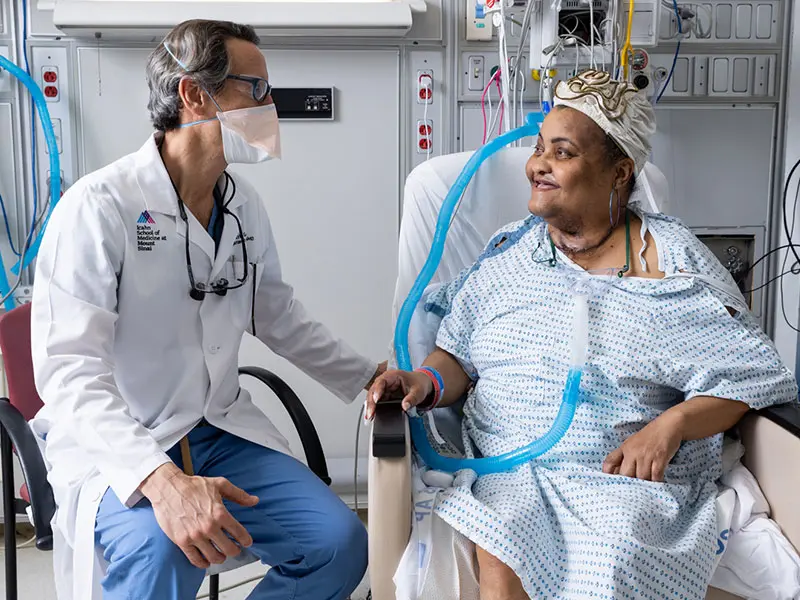
Dr. Genden checks in with Ms. Sein following her historic surgery.
This historic case launches Mount Sinai’s Trachea Transplant Program and lays the foundation for treating patients worldwide. As the team continues to closely monitor Ms. Sein’s progress, what they learn will inform future protocols. Dr. Genden, who is the Isidore Friesner Professor and Chair of Otolaryngology – Head and Neck Surgery for Mount Sinai Health System, looks forward to sharing his findings with colleagues at national meetings and conferences to help accelerate the field.
“I want other surgeons to know that this procedure is not too technically difficult,” he says. “Anyone trained in microvascular surgery can offer this solution to patients who come to them with no hope.”
Physicians often hear immunosuppressants are fraught with problems. However, Dr. Genden says new techniques make transplantation far less burdensome for patients. Based on what they have seen with the graft beginning to grow into the recipient, he suspects they may be able to stop immunosuppressive therapies altogether one day.
“It is no longer a big cost to be on immunosuppression. This patient is at home taking only two pills a day,” says Dr. Genden. “As we learn more and study new protocols it will only make the time following transplantation even easier.”
Now that the procedure has succeeded, questions have arisen regarding the ideal immunosuppressive regimen, the ideal recipient, and the implications for lung and other types of transplantation. Dr. Genden plans to spend the remainder of his career researching these topics and refining his technique.
“When you are a surgeon, you try to save one life at a time, but when you come up with something like this you have the potential to impact generations,” he says. “I have a responsibility now to return to the lab, work on protocols, and commit myself to advancing the science. With the clearance of vascularized composite allograft transplants, this could become a relatively common procedure. A whole new world is going to open up in organ transplantation.”
Featured

Eric M. Genden, MD, MHA, FACS
Professor and Chair of Otolaryngology – Head and Neck Surgery