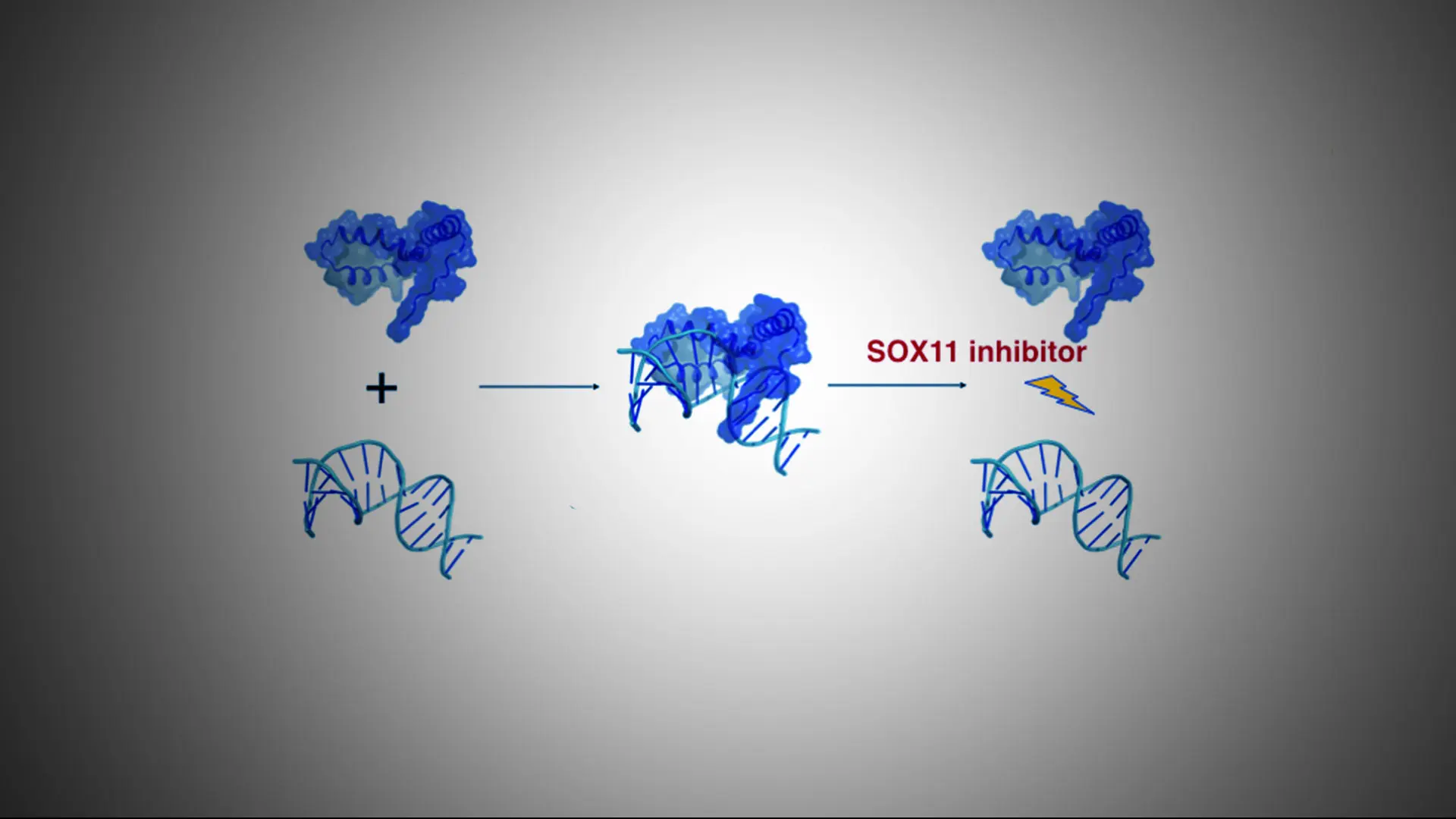
SOX11, the oncogene expressed in up to 90 percent of patients with mantle cell lymphoma (MCL), has handed drug developers an attractive therapeutic target. The challenge, however, is that SOX11—a transcription factor that binds to DNA and acts as a master switch to turn genes off and on—is generally considered undruggable.
Recently, researchers at The Tisch Cancer Institute discovered how to overcome this long-standing hurdle by employing a family of small-molecule inhibitors of SOX11 that are toxic to MCL tumor development. The breakthrough, described in the July 12, 2021, issue of Clinical Cancer Research, could potentially lead to a novel class of therapeutic agents for MCL, a disease that is highly resistant to existing treatments.
“Until now, no effective small-molecule inhibitor had been identified for therapeutically targeting this oncogene,” says the study’s senior author, Samir Parekh, MD, Professor of Medicine (Hematology and Medical Oncology) at the Icahn School of Medicine at Mount Sinai. “We discovered three structurally related compounds that are able to bind to the oncogene, perturb its interaction with DNA, and, through their anti-MCL cytotoxicity, actually kill lymphoma cells with remarkable efficiency.”
SOX11 has been a major obstacle in identifying treatments for MCL.
MCL represents approximately 6 percent of all cases of non-Hodgkin’s lymphoma, the most common hematological malignancy worldwide. Despite advances in chemotherapy and immunotherapy, MCL patients have a median survival of seven to eight years, and exhibit a
continuous pattern of relapse to therapies such as ibrutinib, a small-molecule drug approved by the U.S. Food and Drug Administration for MCL and chronic lymphocytic leukemia. SOX11 has been a major obstacle in identifying compounds that could overcome cellular resistance to treatment.
After screening more than 12 million compounds, Mount Sinai researchers found a family of three that fit into a pocket on the SOX11 surface as a way to interfere with DNA binding, thereby blocking the mechanism by which MCL develops.
In ex vivo studies, one of those three compounds showed cytotoxic synergy with ibrutinib. Ibrutinib binds to BTK, a protein that is part of a signaling cascade, which triggers the malignant transformation of B lymphocyte cells into MCL. In collaboration with their colleagues at The Ohio State University, the Mount Sinai team also showed that the drug is active against ibrutinib-resistant tumor cells.
“These small-molecule inhibitors could also be useful for understanding the pathogenesis of other malignancies that can be traced to SOX11, including epithelial ovarian tumors, medulloblastoma, gliomas, and basal-like breast cancer.”
- Samir Parekh, MD
While ibrutinib acts independently to fight MCL, the researchers believe that the agent, in combination with a SOX11 inhibitor, could be particularly potent against ibrutinib-resistant cancerous cells.
“These small-molecule inhibitors could also be useful for understanding the pathogenesis of other malignancies that can be traced to SOX11, including epithelial ovarian tumors,
medulloblastoma, gliomas, and basal-like breast cancer,” says Dr. Parekh. “Many transcription factors exist in a variety of tumors that could be targeted by scientists. What we’ve demonstrated through our work is that there is, indeed, an effective way to make them druggable.”
Featured

Samir Parekh, MD
Professor of Medicine (Hematology and Medical Oncology)