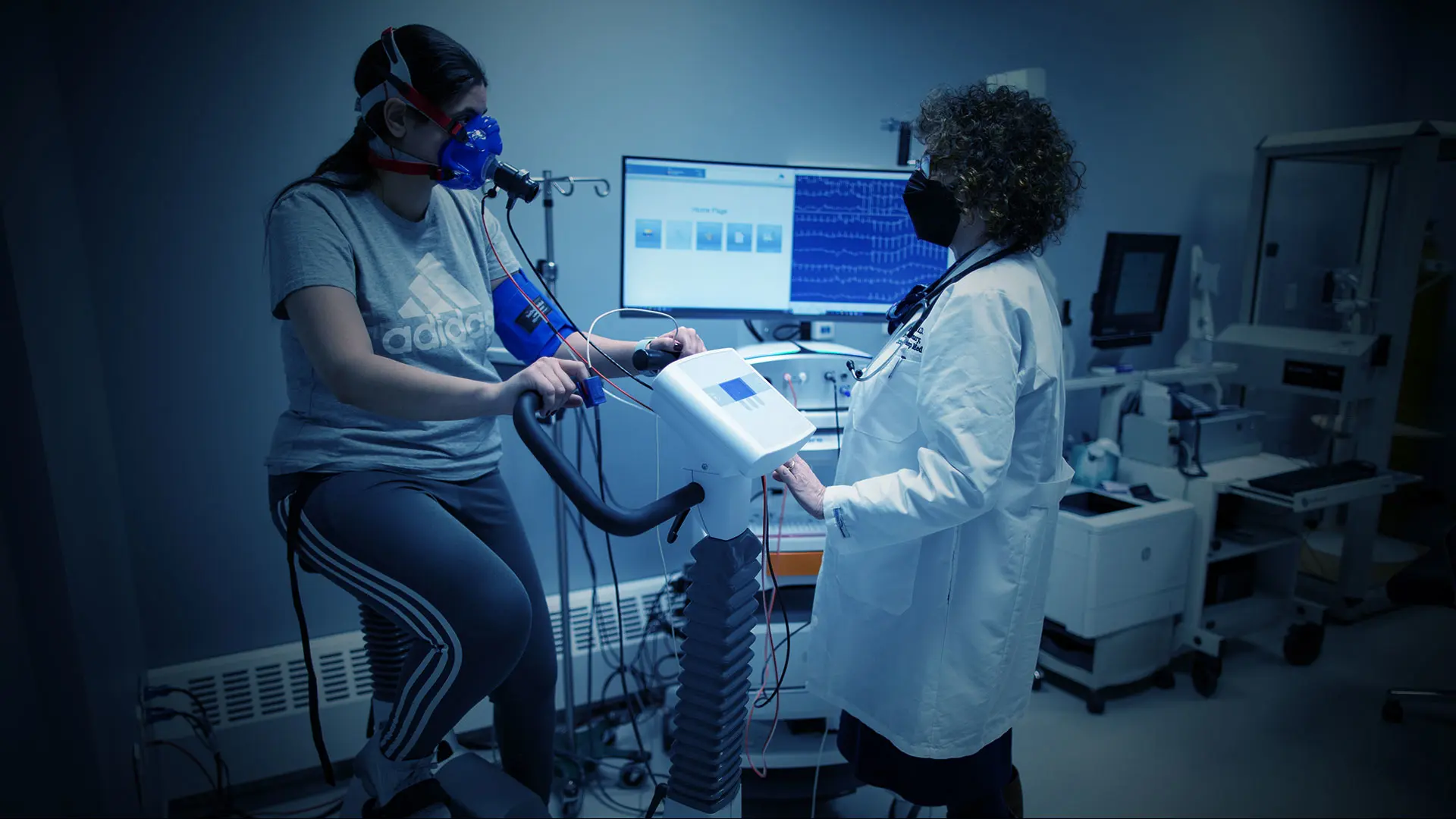
When patients with unexplained shortness of breath have undergone an extensive array of X-rays, spirometry, echocardiogram, and pulmonary function tests without any answers as to the cause of their condition, they are referred to Mount Sinai’s Helena Schotland, MD, to break the test-and-imaging cycle.
As director of Mount Sinai’s exercise physiology program, Dr. Schotland has set a goal of gaining the insights necessary to make a definitive diagnosis in just 10 minutes.
“We have a stationary bike set up, and we want them to hit anaerobic threshold within that time limit,” says Dr. Schotland, Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine at Mount Sinai. “How we do that will be different for an older patient versus a marathoner or elite athlete, but we push them really hard to get all the information we need.”
Getting things up to speed quickly is something of a specialty for Dr. Schotland. Charged with reinvigorating an exercise physiology program that was essentially dormant due to the COVID-19 pandemic, she has given it a reboot. Sleek state-of-the-art hardware has been introduced, software upgrades have been made, and technicians have undergone extensive training on the new system to facilitate testing.
But the biggest boost for the refurbished program may be Dr. Schotland’s expertise. She first became interested in pulmonary function tests and cardiopulmonary exercise during her pulmonary and critical care fellowship at the University of Pennsylvania. Prior to joining Mount Sinai in December 2021, she served as director of the pulmonary function laboratory at the University of Michigan.
“There are very few pulmonologists who are interested enough in exercise testing to make it part of their career,” Dr. Schotland says. “The data that you need to process can be overwhelming and there are not many of us who feel comfortable doing that every day. I have loved it from the moment I heard about it more than 30 years ago, so I think it is a combination of interest and expertise that makes me unique.”
Data for patient diagnoses are gathered using a heart rate monitor, pulse oximeter, and tachograph, all of which are connected to a computer. Patients are also outfitted with a mask that measures their oxygen consumption and carbon dioxide production. Once baseline data are established, patients begin pedaling. As the test proceeds, the resistance they experience is steadily increased using a computer-programmed ramp protocol that is customized based on each patient’s medical history, age, and activity levels.
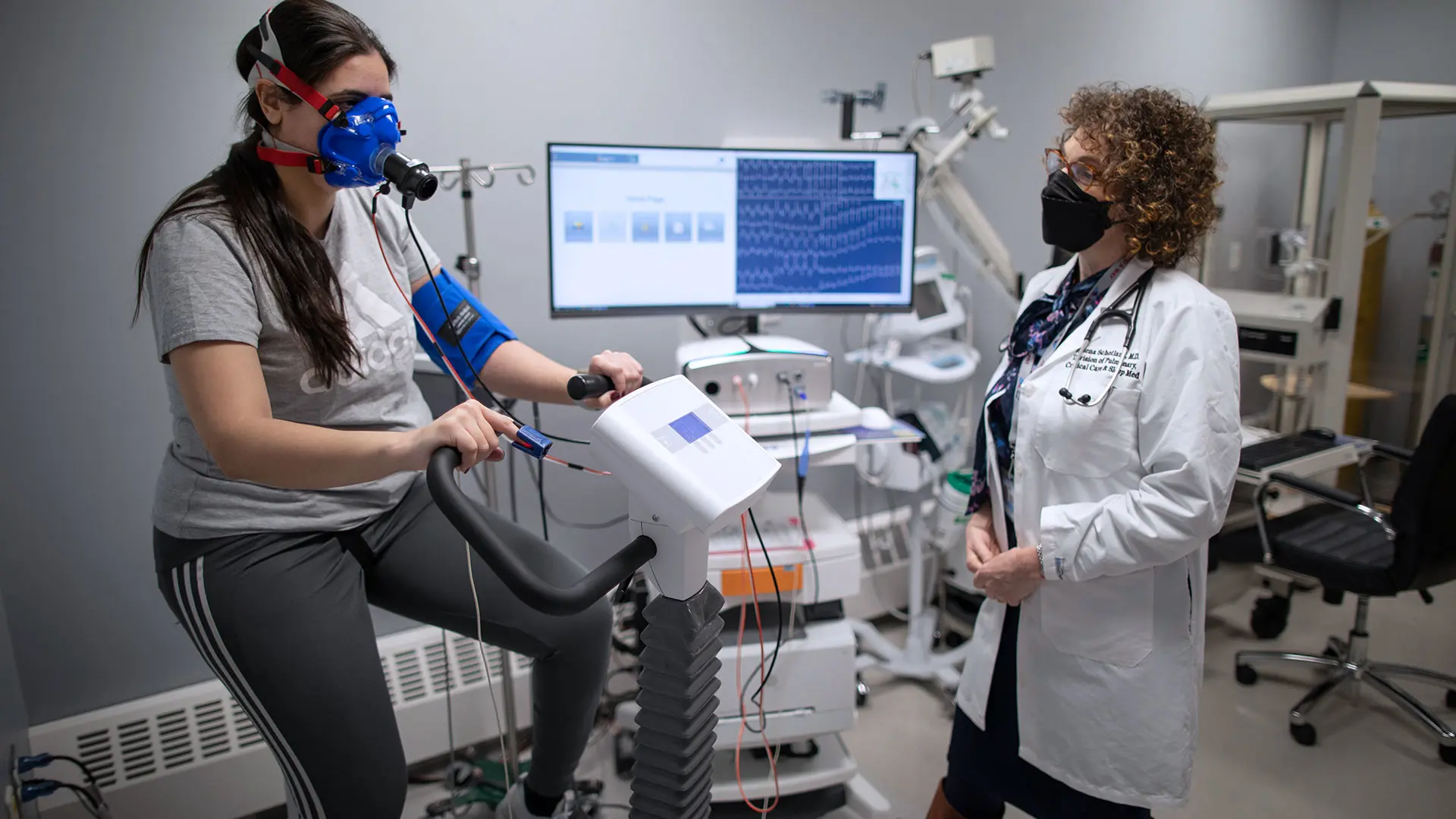
Helena Schotland, MD, uses 10-minute exercise physiology tests to gain the data and insights necessary to diagnose a range of pulmonary diseases.
Although the goal for each patient is to reach anaerobic threshold, that is not always possible. In some instances, patients stop the test due to shortness of breath, leg discomfort, or an inability to continue. In other cases, the team will stop a test if a patient experiences chest pain, heart rhythm abnormalities, or a significant drop in oxygen saturation. “When patients complete or stop the test, they go into recovery, and we monitor them to ensure everything is fine before they are released,” Dr. Schotland says.
Once the attending physician assembles the session data, Dr. Schotland, who partners with Kevin Rurak, MD, a Clinical Instructor of Pulmonary, Critical Care, and Sleep Medicine at Icahn Mount Sinai, begins the detective work, analyzing hundreds of data points in isolation, in context, and against the patient’s medical history. The sheer volume of information can be overwhelming—she likens it to being dropped in the ocean—but the exercise physiology team physicians typically focus first on the patient’s work rate, maximum oxygen consumption, and anaerobic threshold. For cases of exercise limitation, the physician’s report will identify the cause of the limitation and can suggest additional testing and treatment to be considered as appropriate for the patient.
With the refreshed program up and running, Dr. Schotland has been making moves to further enhance it. For one, she will provide additional training to Dr. Rurak, who joined Mount Sinai’s Pulmonology faculty in July 2022 after completing several months of advanced training in pulmonary physiology and cardiopulmonary exercise training at National Jewish Health in the fall of 2021. A training component has also been introduced to equip Mount Sinai pulmonology fellows with the knowledge to interpret exercise tests. Additionally, the program will introduce a more comprehensive and invasive version of the exercise test in which a right heart catheter is used to measure right-sided heart pressures when the patient is at rest and exercising. This would deliver cardiopulmonary hemodynamic insights, thus facilitating Drs. Schotland and Rurak’s ability to make diagnoses in more complex cases.
“Our focus is on maintaining an exercise physiology program of innovation and excellence so that we can provide our patients with answers that make effective treatment of their condition possible,” Dr. Schotland says.
Featured

Helena Schotland, MD
Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine)

Kevin Rurak, MD
Clinical Instructor of Medicine (Pulmonary, Critical Care and Sleep Medicine)