Related Article
Just three years ago, pleural disease diagnosis and management at Mount Sinai Health System involved invasive approaches such as pleural biopsies and pleurodesis performed using video-assisted thoracoscopic surgery. Patients required general anesthesia and hospital admission.
Realizing that many of the patients he sees are too ill to tolerate such procedures, interventional pulmonologist Udit S. Chaddha, MBBS, saw an opportunity to effect positive change.
“Nobody in our division was performing pleuroscopy at the time,” he says. “It is a minimally invasive procedure, and we are able to perform a biopsy or pleurodesis as a 20-minute outpatient procedure using moderate sedation and a single port. Once we introduced pleuroscopy, it resulted in a cultural change that led to Pulmonology being consulted on almost every patient with pleural disease. It also resulted in a dramatic increase in referrals, and that provided the impetus for us to start a formalized pleural disease program.”
Launched in 2020, the Mount Sinai – National Jewish Health Respiratory Institute’s Pleural Service has attracted considerable interest and referrals, resulting in a 100 percent growth in pleural procedures. Dr. Chaddha, the program’s director, attributes that accomplishment, in part, to state-of-the-art equipment, the implementation of patient management protocols, and the comprehensive array of services and expertise available through the program.
“Pleuroscopy is probably the main procedure we do,” says Dr. Chaddha, Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine), and Thoracic Surgery; Associate Program Director of Interventional Pulmonology; and Associate Director of Interventional Pulmonology with the Catherine and Henry J. Gaisman Division of Pulmonary, Critical Care and Sleep Medicine at the Icahn School of Medicine at Mount Sinai.
“We also perform indwelling pleural catheter placement, large- and small-bore chest tubes, thoracentesis, closed pleural biopsies and biopsies of pleural-based or chest wall masses using ultrasound, and pleurodesis. Additionally, we participate in the management of empyema patients, such as decisions on when to administer tissue plasminogen activator and deoxyribonuclease, and in the management of pneumothorax patients, managing them in the acute setting and conducting follow-ups to ensure their care is appropriate.”
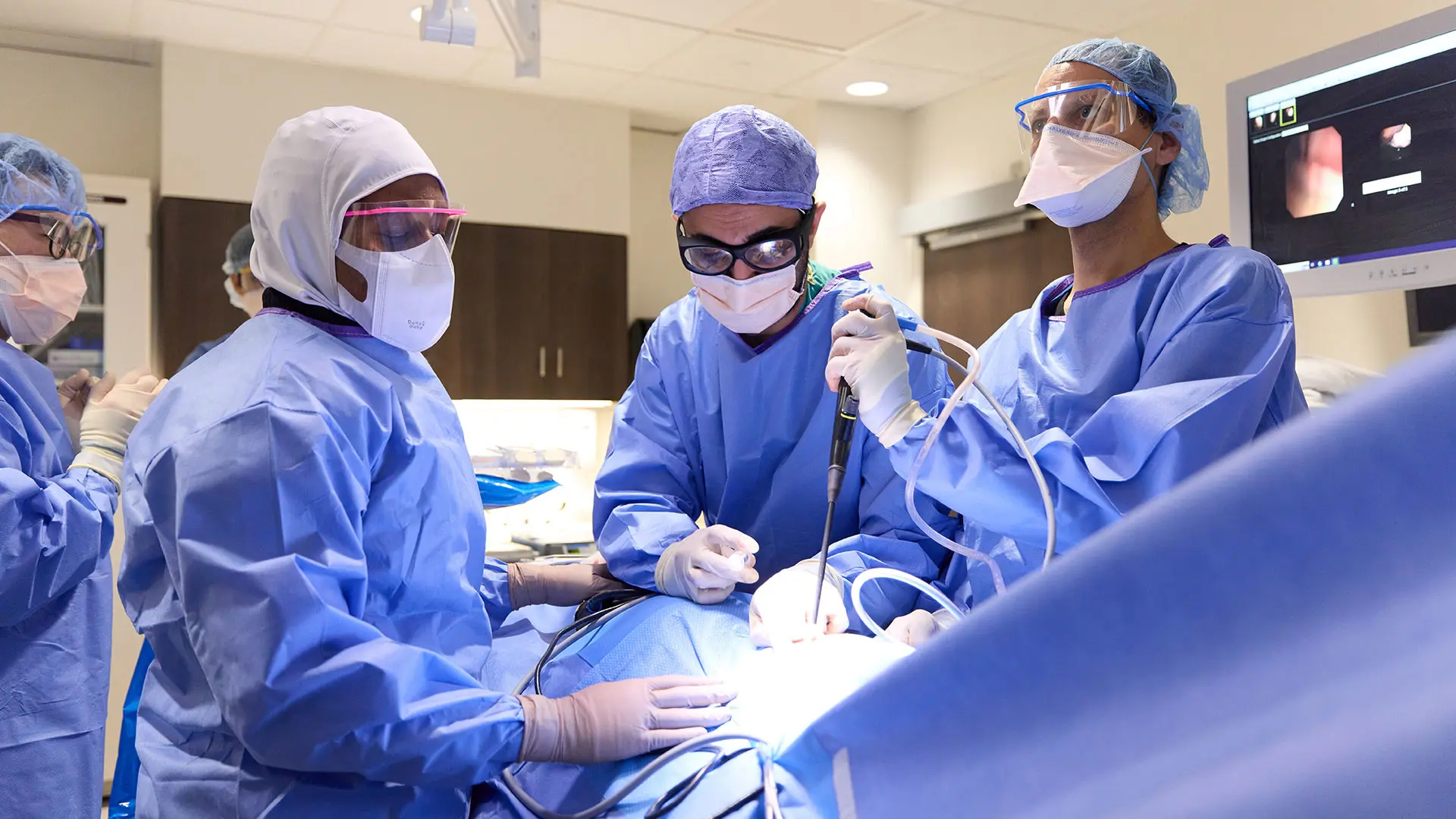
Udit S. Chaddha, MBBS (center), along with assistants Christian Lo Cascio, MD (Interventional Pulmonology fellow; right) and Idayat Brimah, MD (Pulmonary Critical Care fellow; left), and endoscopy technician Bongick Jang (far left), performing a pleuroscopy in the Mount Sinai West endoscopy suite.
The goal of the program is to provide timely delivery of treatment—within minutes for emergent situations and hours for all other cases. A dedicated weekly clinic staffed by Dr. Chaddha; a nurse, Lilibeth Simporios, RN; and a fellow has facilitated that effort, resulting in patients undergoing pleural procedures within one week of referral. Additionally, procedure time is reserved in endoscopy, so that all patients can be attended to without delay.
“It is a set system, which sounds simple, but it enables state-of-the-art care to be the norm here, which is not the case nationwide,” Dr. Chaddha says. “There are very few pleural programs nationwide, as there are only approximately 40 interventional pulmonology fellowship programs. And there are only 400 interventional pulmonologists who are fellowship-trained, which is a requirement for launching a program like this. This means that, for the next decade, it will not be possible for smaller hospitals to offer patients an all-encompassing program.”
Dr. Chaddha anticipates the program will fill that gap through the services it offers and through a dedicated interventional pulmonology fellowship. Led by Timothy Harkin, MD, Associate Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine), and Thoracic Surgery, and Director of Bronchoscopy at Icahn Mount Sinai, the fellowship is offered to one candidate each year. Dr. Chaddha sees other ways that the program can have an impact, such as increased research and clinical trial activity to gain more insights on the pathology of pleural disease and offer more therapeutic options to patients.
“Our goal is to have dedicated fellows and research coordinators in place so that we can increase that activity within the next two to three years,” he says. “That will enable our research efforts to be smoother and faster, and we will be able to recruit more patients and address the unmet need for treatment.”
Featured Faculty and Division Leadership

Udit S. Chaddha, MBBS
Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine), and Thoracic Surgery

Timothy Harkin, MD
Associate Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine), and Thoracic Surgery

Charles A. Powell, MD, MBA
Chief of Pulmonary, Critical Care and Sleep Medicine; Director, Mount Sinai Respiratory Institute