A Mount Sinai physician-scientist, Eugenia Alessandra E. Alleva Bonomi, MD, MSc, is leading the development of two tools to expedite identifying heavy menstrual bleeding (HMB)—an understudied and undertreated condition. The project is part of a multisite program funded by the nonprofit group Wellcome Leap, which awarded Dr. Alleva a contract for this research in 2025.
“HMB is an important issue and leads to chronic blood loss,” says Dr. Alleva, Assistant Professor of Obstetrics, Gynecology and Reproductive Science, and Artificial Intelligence and Human Health at the Icahn School of Medicine at Mount Sinai, noting that one in three women in the United States reports heavy menstrual bleeding. HMB can lead to iron deficiency and iron-deficiency anemia and has also been recently linked with increased heart disease risk. It has a highly negative effect on quality of life. In addition, menstruation can be an indicator of overall health—the reason that the project funded by Wellcome Leap is known as “The Missed Vital Sign.”
“Quantitatively, HMB is defined as losing more than 80 milliliters of menstrual blood per menstrual cycle, but for the purposes of this study, we are viewing it in a more personalized way, as the actual amount of blood loss that has impacts on iron stores at the single-patient level,” Dr. Alleva says. Studies suggest that half of women with HMB do not seek out medical help. When they do, it can take about three years to develop a diagnosis. “There are several reasons for this,” Dr. Alleva says. “First, menstruation specifically and women’s health issues in general have been very stigmatized historically, so many people, including scientists, are reluctant to discuss it. Second, menstrual disorders are often underestimated by clinicians, even though, for example, very severe HMB can lead to dramatic consequences, such a hemorrhage and death. The third reason is that the menstrual physiology and pathology have been studied primarily in terms of reproduction and infertility, not overall health or quality of life.”
“Menstrual physiology and pathology have been studied primarily in terms of reproduction and infertility, not overall health or quality of life.”
Eugenia Alessandra E. Alleva Bonomi, MD, MSc
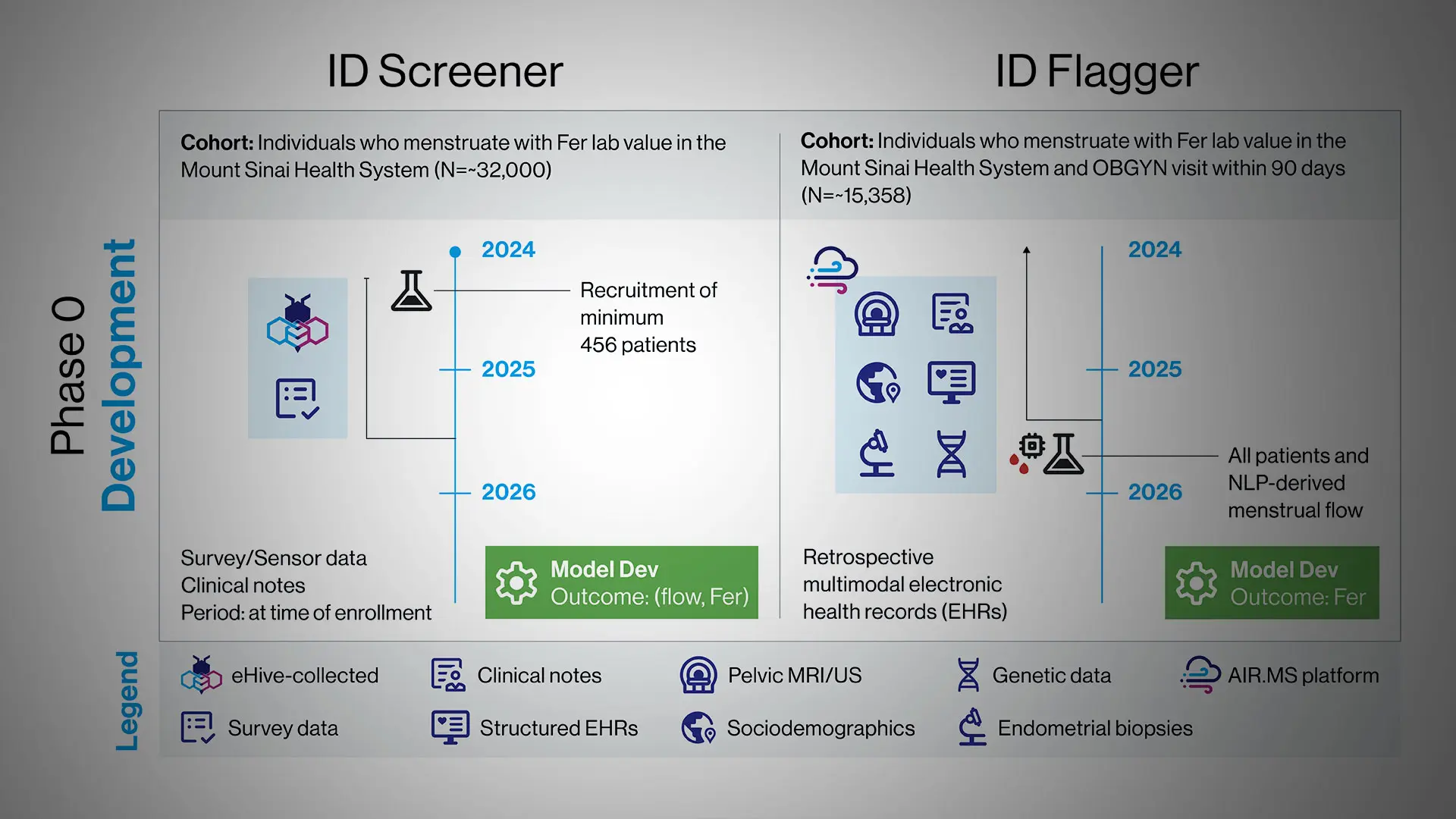
Dr. Alleva is developing two screening tools, one for patients and the other for physicians. The patient-facing screening tool will enable women to assess their risk of HMB and associated iron deficiency in the privacy of their homes. It will rely on a survey that is under development and on data already accessible via smartphones and wearable devices. The tool will identify predictors of HMB at levels that are likely to cause iron depletion, by modeling menstrual flow and ferritin concentration. “These data, including oxygenation, physical activity, and heart rate, are available on every smartphone in the world,” Dr. Alleva says.
The second tool would enable clinicians to identify patients at risk for HMB-associated iron deficiency and iron deficiency anemia. It will use electronic health record data and, when available, additional information including genetic information, imaging and pathology data, such as pelvic imaging studies and digitized endometrial biopsies. The tool aims to flag at-risk patients and prompt clinicians to investigate the presence of HMB. If HMB is present, physicians can proceed with appropriate diagnostics and treatment.
Both tools aim to be scalable across different ages, geographies, cultures, abilities, and demographics. “I’m excited to use machine learning research to have a real impact on patients’ lives,” Dr. Alleva says.
In announcing its program, Wellcome Leap said, “We need to close the gap in our biological understanding of the fundamental mechanisms that occur when the uterine lining breaks down, sheds, and repairs at menstruation. In this program, we intend to demonstrate the advances in women’s health that are possible when menstruation is treated as a vital sign. Our goal is to reduce the time it takes a woman to get effective treatment for HMB more than tenfold—from five years to five months.”
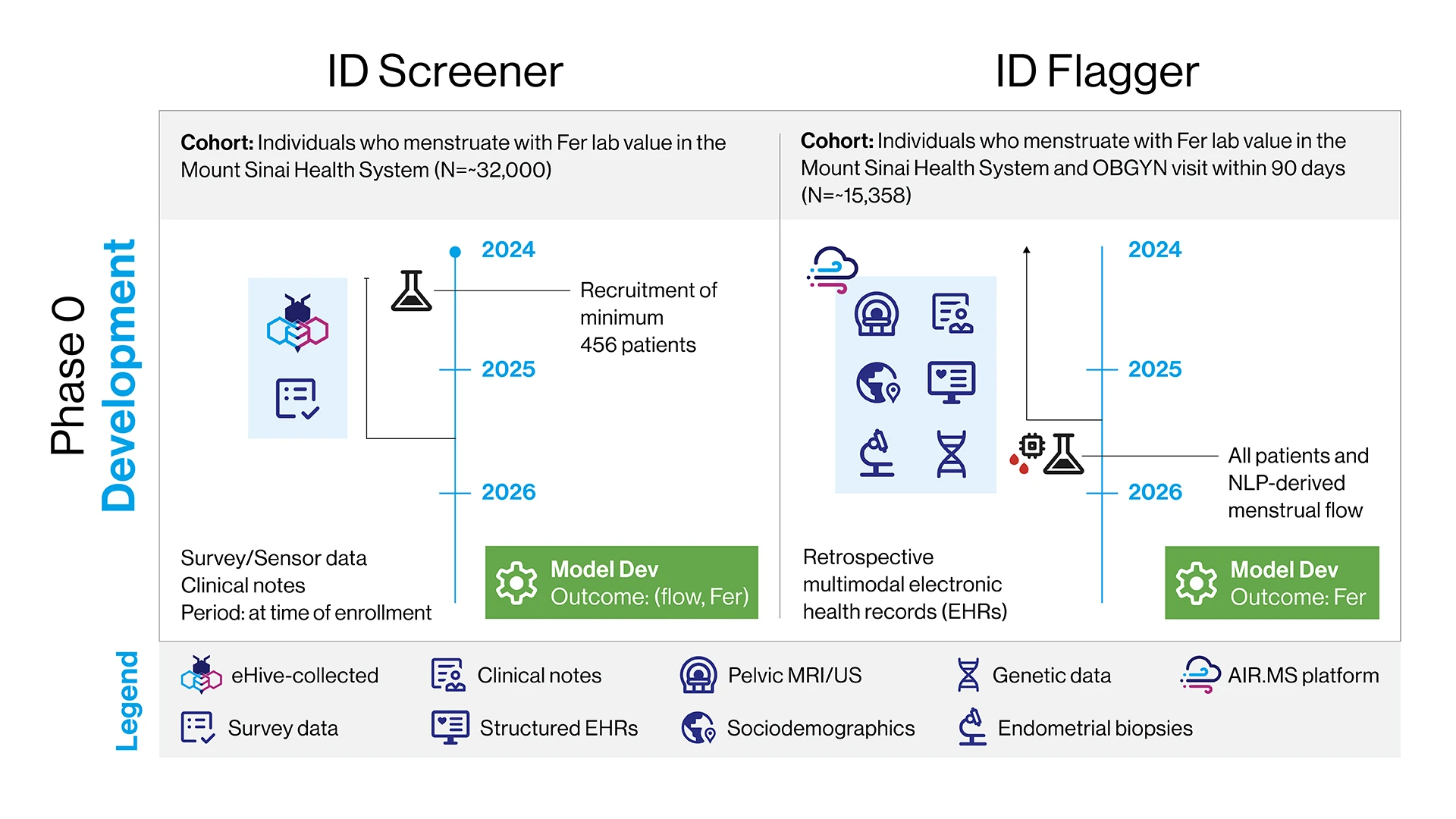
In Phase 0, the models will be developed independently using retrospective cohorts tailored to their respective inputs. This phase includes dataset assembly, recruitment (for the ID Screener), creation of preprocessing pipelines (e.g., for sensor alignment and image extraction), and training, comparison and refinement of multiple model architectures.
The Mount Sinai effort is 1 of 13 research initiatives taking place in The Missed Vital Sign program, which are based at institutions around the globe. Participating researchers will hold periodic meetings, starting in spring 2025, to formalize the process for collaboration and data-sharing, enabling each study to produce more robust results.
In addition to The Missed Vital Sign project, Wellcome Leap is funding a range of women’s health research, including a Mount Sinai study of the relationship between estrogen decline, insulin resistance, brain aging, and Alzheimer’s disease, being conducted by Natalie Rasgon, MD, PhD, Professor of Psychiatry at Icahn Mount Sinai.
This research is funded under another project—Cutting Alzheimer’s Risk through Endocrinology (CARE). Dr. Rasgon’s team is using multimodal neuroimaging, cognitive testing, and in vivo assessment of neuronal biomarkers of neurodegeneration in deep phenotyping women who undergo surgical menopause. The objective is to identify biomarkers and therapeutic targets that can enable early intervention and effective risk mitigation for Alzheimer’s dementia.
“It's an exciting opportunity to see some of what’s happening in individuals within the in vivo model.,” Dr. Rasgon says. “There are plenty of animal and in vitro models of estrogen effects in the brain that have been acquired over the past few decades, yet understanding brain reaction to abrupt discontinuation of exposure to endogenous estrogen remains elusive.”
Featured

Eugenia Alessandra Alleva Bonomi, MD, MSc
Assistant Professor of Obstetrics, Gynecology and Reproductive Science, and Artificial Intelligence and Human Health, Icahn School of Medicine at Mount Sinai

Natalie Rasgon, MD, PhD
Professor of Psychiatry, Icahn School of Medicine at Mount Sinai