A multidisciplinary team at Mount Sinai is conducting the first large-scale prospective study to examine the impact of COVID-19 infection, and the immune response, during pregnancy on maternal and child outcomes. The study, known by the team as “Generation C,” is funded by a $1.8 million contract from the Centers for Disease Control and Prevention and is expected to be conducted through May 2022.
The study has an important public health mission—informing clinicians and patients about trimester-specific risks associated with contracting SARS-CoV-2, the virus that causes COVID-19, during pregnancy. The Mount Sinai team will also examine the extent to which COVID-19 disproportionately impacts pregnant women from underserved communities, and how stress may mediate the effects of COVID-19.
“Early in the pandemic, there were reports that women who tested positive during delivery might have a higher risk of birth complications,” said a co-investigator, Veerle Bergink, MD, PhD, Professor of Psychiatry, and Obstetrics, Gynecology and Reproductive Science, Icahn School of Medicine at Mount Sinai. “We want to know, not only for symptomatic women but also for the asymptomatic women, what exposure to COVID-19 means for your obstetric outcomes and for your baby.”
“We are looking at the impact and timing of SARS-CoV-2 infection and the development of COVID-19 on acute and severe complications.”
Joanne Stone, MD
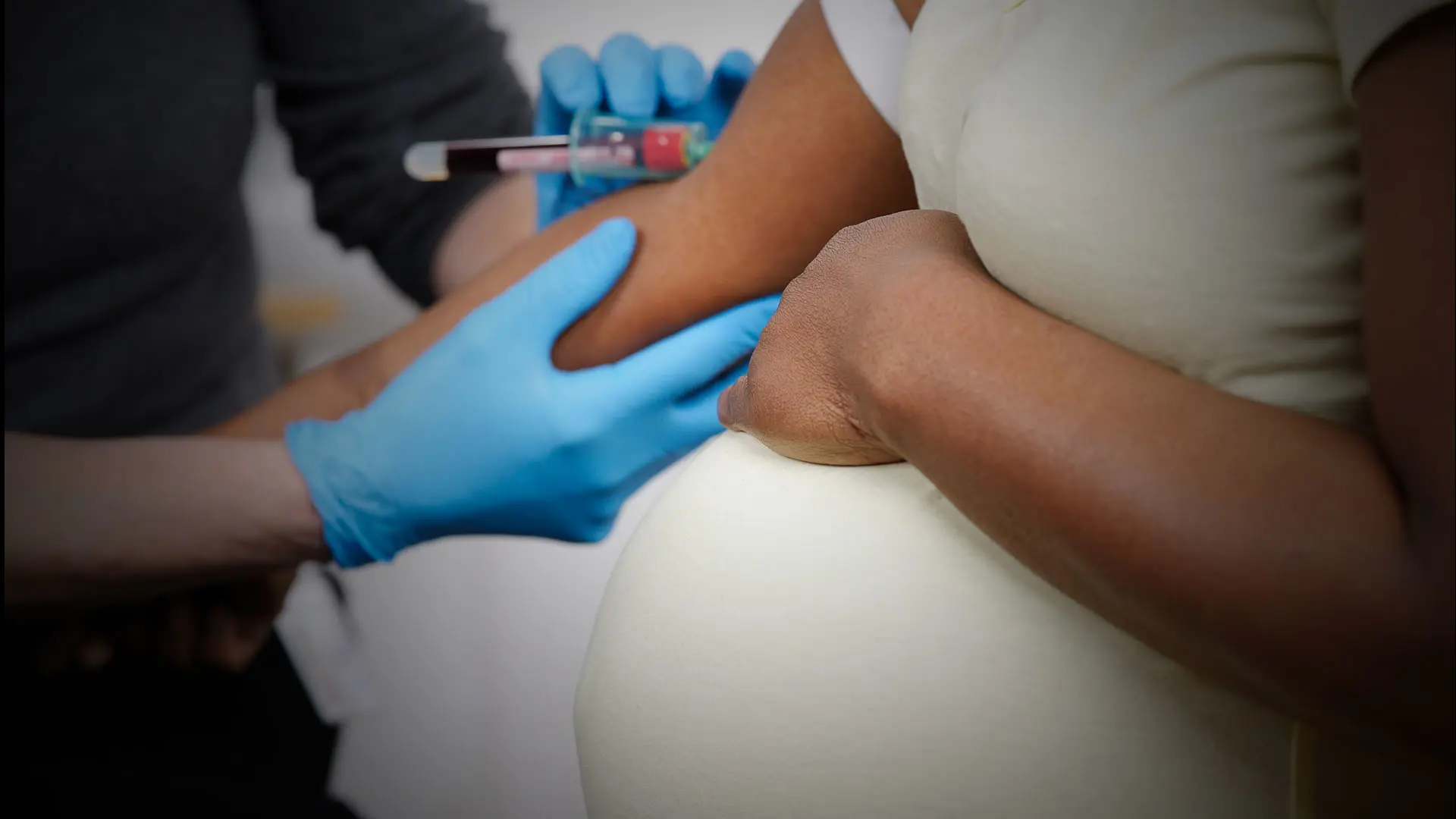
The research team intends to study a cohort of 3,000 pregnant women at The Mount Sinai Hospital and Mount Sinai West, with more than 2,500 enrolled as of May 2021. “For the women involved, this is really a simple study,” Dr. Bergink said. “It’s basically only giving an extra tube of blood.”
Researchers are examining plasma samples drawn as part of routine care at each trimester of pregnancy in all pregnant women at the two hospitals. Samples are tested for the immunoglobulin M and immunoglobulin G antibodies to SARS-CoV-2 at each trimester of pregnancy and at delivery. The hypothesis is that the level of inflammatory host response to SARS-CoV-2 exposure is related to the impact of the infection on maternal and child outcomes, and that timing is crucial.
The study is examining the subjects’ electronic medical records, obtaining data on obstetric complications, miscarriage, premature rupture of membranes, delivery type, maternal ICU admissions, acute respiratory distress syndromes, sepsis, and maternal death. In addition, the team is extracting data on fetal growth and neonatal outcomes, including birth weight, preterm birth, neonatal morbidities, neonatal intensive care admissions, congenital malformations, and fetal and neonatal death.
“We are looking at the impact and timing of SARS-CoV-2 infection and the development of COVID-19 on these acute and severe complications,” said co-principal investigator Joanne Stone, MD, Professor of Obstetrics, Gynecology and Reproductive Science, Icahn School of Medicine, and Director of Maternal Fetal Medicine, Mount Sinai Health System. “The aim is to investigate whether SARS-CoV-2 infection and a strong inflammatory host response are related to preterm delivery and neonatal morbidity.”
Another aim of the study is to examine the extent to which COVID-19 disproportionately impacts pregnant women from underserved communities. This part of the study is taking full advantage of the diversity of Mount Sinai’s patient population. “We have women from the affluent Upper East Side of Manhattan, from the Bronx, from Harlem,” said co-principal investigator Siobhan Dolan, MD, MPH, Vice Chair for Research and Director of Genetics and Genomics, Department of Obstetrics, Gynecology and Reproductive Science, and Co-Director of the Blavatnik Family Women’s Health Research Center. “The ethnic and socioeconomic diversity of our patients means that we do a very good job of reflecting the United States population.”
Finally, the researchers are investigating how maternal stress related to the COVID-19 outbreak is associated with adverse pregnancy and neonatal outcomes. In addition to data collected at Mount Sinai, the team is leveraging an ongoing prospective cohort study of 1,320 subjects in the Netherlands, in which blood samples are drawn at each trimester of pregnancy and online mental health questionnaires in each trimester are distributed. Blood samples and data (50 percent collected before, and 50 percent during the pandemic) will be sent to Mount Sinai for analysis. Intrauterine exposure to maternal stress has been associated with adverse child outcomes, including preterm birth and low birth weight, and various long-term effects.
The World Health Organization classifies pregnant women as at high risk for serious COVID-19-related morbidity and mortality. Pregnant women are seen as particularly susceptible to respiratory pathogens because they are in a state of immune tolerance and are relatively intolerant to hypoxia. The Mount Sinai study was proposed in response to a CDC call for research that will bolster the very limited data now available on the effects of SARS-CoV-2. It was designed by Dr. Bergink and Elizabeth Howell, MD, MPP, who is now Chair of Obstetrics and Gynecology at the Perelman School of Medicine at the University of Pennsylvania.
“We are starting to see vaccines, which is important,” Dr. Bergink said. “But this virus will be among us for a while, and it is good to have real-life data on the effects of COVID-19, especially in vulnerable groups, like pregnant women and high-risk populations.”
Featured

Joanne L. Stone, MD, MS
Chair and Professor of the Raquel and Jaime Gilinski Department of Obstetrics, Gynecology and Reproductive Science

Noël Strong, MD
Assistant Professor of Obstetrics, Gynecology and Reproductive Science