Exposure to ionizing radiation during fluoroscopic guidance has long been considered an unavoidable occupational hazard for urologists.
A Mount Sinai physician recognized as a pioneer for his advanced research and treatment of urinary stone disease has confronted the issue head-on with a novel technique for removing renal stones that dispenses entirely with fluoroscopy, as well as with the ureteral access sheath and post-operative stenting. The new approach offers protection for not just urologists, but for their patients and surgical staff.
Appropriately named NoFUSS-RIRS (no fluoroscopy (F), ureteral sheaths (US), or stents (S) during retrograde intrarenal surgery) by its creator, Mantu Gupta, MD, Professor of Urology at the Icahn School of Medicine at Mount Sinai, the procedure is being used successfully for the vast majority of the nearly 900 stone procedures done annually by surgeons at the Department of Urology. A comprehensive study evaluating the NoFUSS approach was recently reported in World Journal of Urology. Two tables below show some of the data.
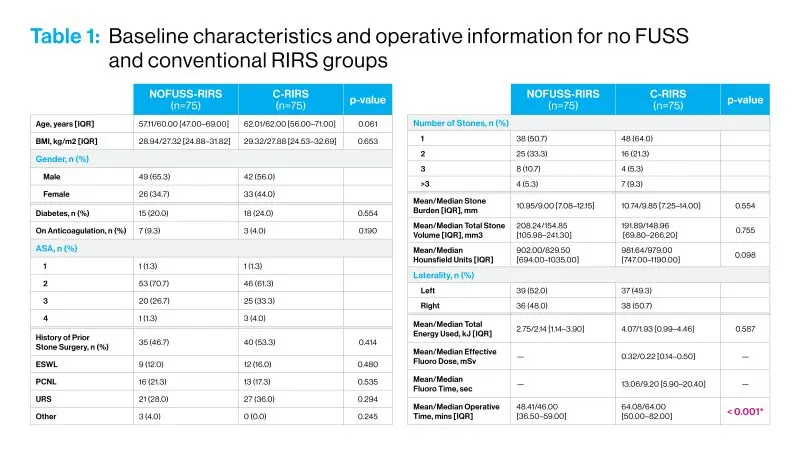
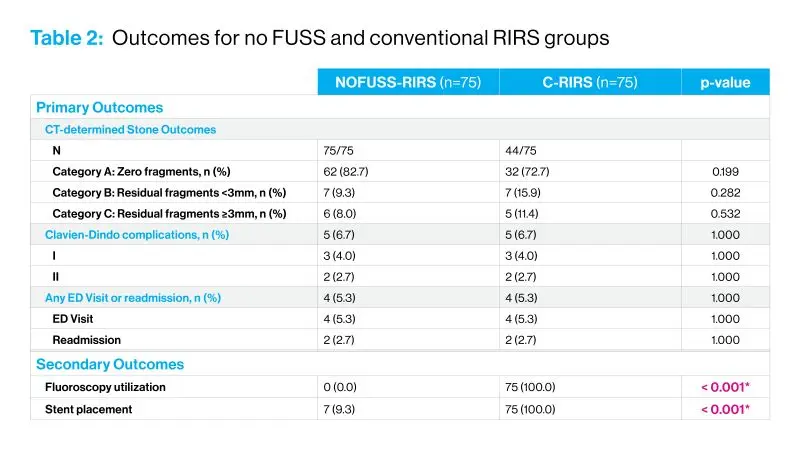
“While the danger of radiation exposure has been identified as a critical issue for the field, our study is among the first to critically assess a surgical protocol that actually omits not just fluoroscopy, but use of sheaths and stent placement,” says Dr. Gupta, who is Site Chair of Urology at Mount Sinai West and Mount Sinai Morningside. “We find that stone-free rates from NoFUSS were comparable to traditional surgery and significantly reduced radiation exposure to patients and OR staff, as well as reduced operating room time and associated costs, could be achieved.”
“We shouldn’t become so complacent that we do things strictly by the way we were taught years ago,” says Mantu Gupta, MD, Professor of Urology at the Icahn School of Medicine at Mount Sinai. “If there’s a way to perform a standard procedure [such as] RIRS that’s better for the patient and better for the surgeon in terms of safety and outcomes, then we should be actively pursuing it.”
Retrograde intrarenal surgery (RIRS) remains a common treatment for urinary stones less than 2 cm due to its high stone-free rates. RIRS is typically performed with fluoroscopic guidance, however, a growing source of concern for urologists as the harmful effects of scatter radiation exposure have become more widely known. Consequently, there has been a growing movement in the field to minimize the use of fluoroscopy during uncomplicated stone excision.
Dr. Gupta has taken that effort to a new level through No-FUSS (fluoroscopy, ureteral sheaths, or stents)-RIRS, which not only eliminates fluoroscopy but further streamlines the procedure by avoiding use of a ureteral access sheath, thereby reducing the potential risk of ureteral wall injury. No less important, No-FUSS-RIRS significantly reduces the need for stent placement, which has been associated with increased pain and lower urinary tract symptoms among patients, resulting in diminished quality-of-life scores. Despite those downsides, as many as 90 percent of patients in the United States still receive a stent following ureteroscopy.
“Because surgeons no longer have to spend time stenting or checking X-rays, No-FUSS reduces OR time and operative cost,” says William Atallah, MD, MPH, Associate Professor Urology at the Kidney Stone Center at Mount Sinai, who now uses the procedure for most of his stone surgeries. “We’ve found we can get the same stone-free rates while being less invasive and using smaller instruments. And the benefits are also considerable for patients, who are exposed to less ionizing radiation and a shorter and more comfortable recovery period following their surgeries.”
Mastering NoFUSS requires a learning curve for surgeons. The Department of Urology has paved the way by teaching residents the fundamentals of the technique early in their careers, a strategy that instructors report leaves them quite comfortable in the OR.

“We’ve found we can get the same stone-free rates while being less invasive and using smaller instruments," says William Atallah, MD, MPH, Associate Professor of Urology.
“They get such good tactile feedback that by the time they graduate they know exactly if they’re in the right spot or not during surgery based on how the guidewire feels and how the ureteroscope feels,” says Dr. Atallah.
Advancing the science and practice of urinary stone removal is nothing new at Mount Sinai. Under the leadership of Dr. Gupta, the Department converted percutaneous nephrolithotomy for large stones into a totally tubeless outpatient procedure, performed with the help of ultrasound guidance in place of X-ray or fluoroscopy to facilitate access. Indeed, ultrasound allows surgeons to watch the needle enter the kidney and place it precisely so that it causes the least amount of bleeding and allows for extraction of all stones through one tract instead of multiple tracts.
Dr. Gupta’s message to other urologists based on his years of experience is that doctors should continue to push for new innovations.
“We shouldn’t become so complacent that we do things strictly by the way we were taught years ago,” he says. “If there’s a way to perform a standard procedure [such as] RIRS that’s better for the patient and better for the surgeon in terms of safety and outcomes, then we should be actively pursuing it.”