In their published work, the researchers, led by Saadi Ghatan, MD, and Fedor Panov, MD, discuss minimizing complications and streamlining RNS system implantation at centers beginning to using this approach.
Approval of a responsive neurostimulation (RNS) system by the U.S. Food and Drug Administration (FDA) in 2013 was a paradigm shift in neuromodulation for epilepsy, but the lack of sufficient data since then has stalled regulatory consent in patients younger than 18. The Mount Sinai Health System, the world’s leading center of RNS utilization in children, has taken a significant step toward closing that information gap with a new study assessing the safety and efficacy of RNS in youngsters with drug-resistant epilepsy (DRE).
Though the prognosis for children with epilepsy is generally favorable, as many as a third develop DRE, in which case resection or laser interstitial thermal therapy may aid in seizure control. Neither, however, is recommended for patients with multiple seizure foci, a seizure
focus in an eloquent area, or poor delineation of the epilepsy network. That created a real need for neuromodulatory treatments like the RNS® System (from NeuroPace Inc.), which was approved as an adjunctive therapy for adults with drug-resistant partial-onset seizures with no more than two epileptogenic foci.
100
the number of RNS devices implanted for epilepsy by Mount Sinai
Mount Sinai reached a major milestone with the placement of its 100th responsive neurostimulator for epilepsy (second in the world) in a 35-year-old man.
In 2015, Mount Sinai implanted the system in the youngest patient ever, a 14-year-old boy who had failed four prior epilepsy surgeries and more than 15 antiepileptic medications, as well as a 9-year-old girl whose seizures emanated from her speech and motor area. The team went on publish that experience, and since then has achieved many other firsts by using RNS in children with Rasmussen encephalitis, a rare disorder that previously was treatable only through hemispherotomy, Tuberous Sclerosis, Lennox Gastaut Syndrome (Annals of Clinical and Translational Neurology 2020), and epilepsy associated with autism.
On Tuesday, September 15, 2020, Mount Sinai reached a major milestone with the placement of its 100th responsive neurostimulator for epilepsy (second in the world) in a 35-year-old man. Dr. Ghatan, Associate Professor and Chair of Neurosurgery for Mount Sinai West and Mount Sinai Morningside, and Director of the Pediatric Neurosurgery Program for the Mount Sinai Health System, and his team have become world-renowned for their groundbreaking work.

Left and Right: Techniques for lead placement during RNS system implantation into the
skull.
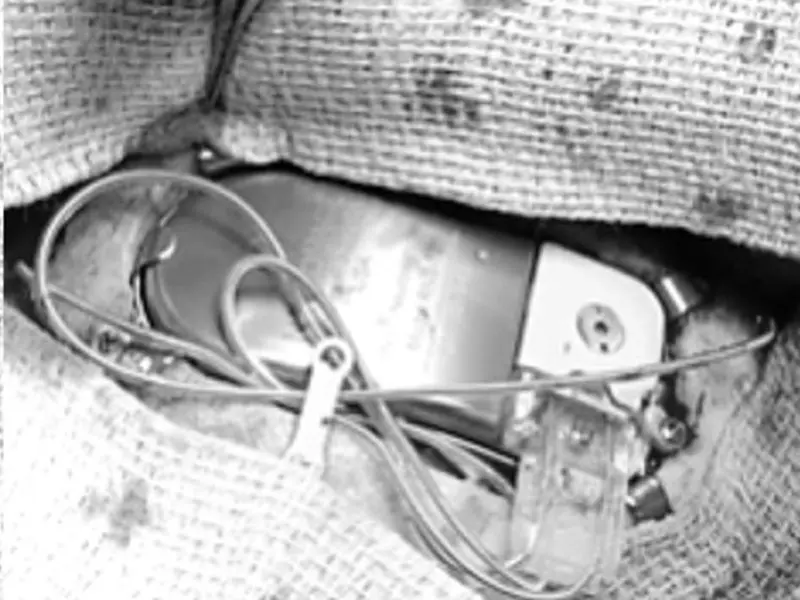
Left and Right: Techniques for lead placement during RNS system implantation into the
skull.
Above: Techniques for lead placement during RNS system implantation into the
skull. Left: To avoid wound problems, the 'legs' of the ferrule were bent so that they were closer to the screw hole to allow the ferrule to sit deeply in the skull. Right: A demonstration of the method used to place backup leads into a small trough between the skull and the sides of the ferrule, with application of a dog bone to keep the leads in place. While there is a recommendation to avoid wires over the neurostimulator, the true no-go area is the tan connector cover. In our experience, we have not seen interference with a mild overlap of wires over the metallic casing.
Review of a planned laser trajectory as it is advanced toward the epilepsy focus target.
“Children with drug-resistant epilepsy represent the toughest cases, and we were able to demonstrate in our study of patients—some as young as seven and eight—the safety and efficacy of responsive neurostimulation,” says lead author Dr. Panov, Assistant Professor of Neurosurgery, and Director of the Adult Surgical Epilepsy Program at The Mount Sinai Hospital. “Seizures became less frequent and less difficult for the child to handle, and we observed that, thanks to the neuroplasticity, it seems that the young brain learns together with the device to fight seizures better over time.”
More than 1/2 of patients had a ≥75% reduction in seizure frequency.
Mount Sinai’s study of 27 patients under 18 (Journal of Neurosurgery: Pediatrics Volume
26 Issue 5 (2020) (thejns.org), found a significant decrease in seizure frequency after RNS system implantation, with more than half of patients experiencing a 75 percent or greater reduction, and no patient showing a worsening of seizures. In addition to its therapeutic benefits, there were no postoperative hematomas, strokes, or RNS system malfunctions, though three patients developed infections, with one successfully treated with antibiotics only, another requiring a partial explant to maintain the therapy, and the third patient needing a full explant of the system.
Dr. Panov also cites the quality of life improvements that often accrue to patients from the procedure. “The greatest problem we hear from all patients with epilepsy is the unpredictability of seizures,” he says. “By significantly decreasing their frequency and making them more manageable when they do occur, RNS can make a huge difference in the quality of their daily lives.”
Dr. Panov is a paid lecturer for NeuroPace, Inc., and Zimmer Biomet.
Featured

Saadi Ghatan, MD
Professor of Neurosurgery, and Pediatrics

Fedor Panov, MD
Assistant Professor, Department of Neurosurgery; and Director, Adult Surgical Epilepsy Program, The Mount Sinai Hospital
