As a surgical fellow 13 years ago, Patricia Sylla, MD, helped develop an innovative approach to low-lying rectal tumors known as transanal NOTES (Natural Orifice Translumenal Endoscopic Surgery) rectosigmoid resection. Later renamed transanal total mesorectal excision (taTME), the technique is now being practiced worldwide. In the absence of long-term results and data from randomized trials, however, questions remain about its safety and effectiveness compared to laparoscopic surgery, and about the level of training and procedures needed by surgeons to ensure proficiency in this highly specialized procedure.
Dr. Sylla, who was recently named Chief of the Division of Colorectal Surgery at Mount Sinai Health System, expects to soon release preliminary results of an 11-site trial in the United States and Canada that she believes will help confirm the importance of taTME in the rectal cancer surgeon’s armamentarium. The phase 2 trial, for which she is Principal Investigator, began enrolling 100 patients in 2017 but was interrupted by COVID-19. It is the first prospective multicenter study in North America to address the question of oncologic safety and functional results of the minimally invasive transanal technique she helped pioneer.
“Everyone is in agreement that laparoscopy is not the best approach for resecting very low rectal lesions that are threatening the anal sphincters,” says Dr. Sylla, Professor of Surgery at the Icahn School of Medicine at Mount Sinai, who performed the first NOTES rectal cancer resection procedure with collaborators in Spain in 2009 and has since trained hundreds of surgeons worldwide. “Laparoscopy is associated with conversion to open surgery rates ranging from 10 percent to 20 percent, and with low rates of anal sphincter preservation.” Even robotic-assisted surgery did not significantly lower conversion rates or improve oncologic results when compared to laparoscopy in a recent randomized trial, she points out.
The real strength of taTME is its ability to facilitate good-quality oncologic resection while preserving at least part of the anal sphincter complex for tumors that are too difficult for laparoscopy to reach, meaning those abutting or within 1 cm of the sphincters or 6 cm from the anal verge.
Indeed, cases of aggressive rectal tumors that have not completely responded to chemoradiation and threaten the anal sphincter have become the bulk of Dr. Sylla’s practice at Mount Sinai. Unless the tumor has completely invaded the sphincter, at least partial sphincter preservation is possible with taTME. As a result, a notable reduction in the rate of abdominoperineal resections (APR), the removal of the rectum and anus and creation of a permanent ostomy bag, has occurred at institutions that have implemented this approach.
Transanal NOTES rectal cancer resection is actually a hybrid procedure that combines standard laparoscopy and transanal endoscopic surgery to remove the rectum. In actual practice, two surgeons work simultaneously: one performs the more straightforward “upper” part of the rectal resection laparoscopically while the transanal surgeon performs the “bottom,” or more complex part, of the rectal dissection. Following the resection, the colon is reconnected to the anus.
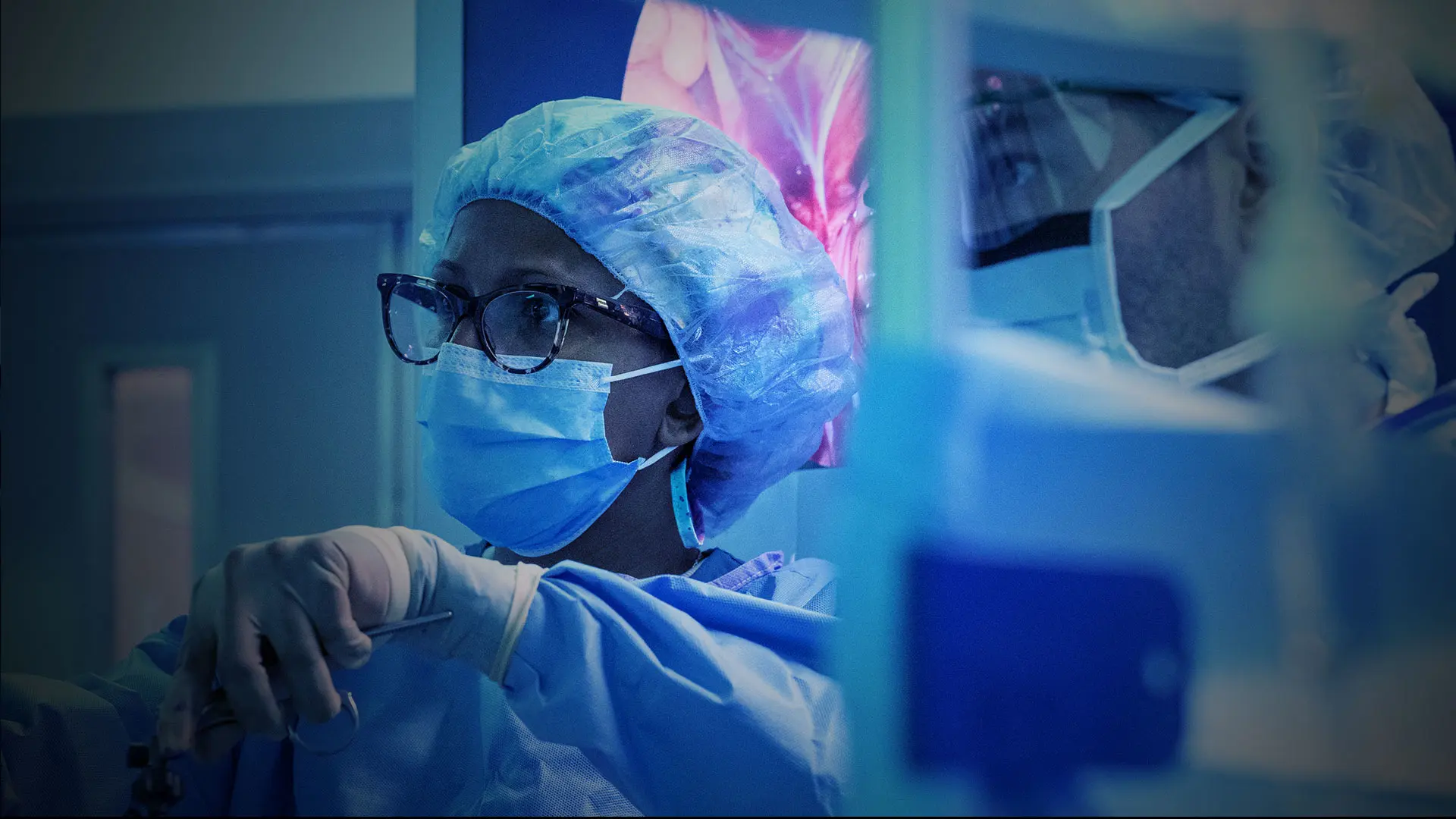
Laparoscopic-assisted transanal total mesorectal excision (taTME) for a low rectal cancer in a male patient.
Dr. Sylla observes that a preliminary analysis of results from the phase 2 trial, conducted entirely across centers of expertise, shows that taTME was associated with good early oncologic results, acceptable morbidity, and only a 2 percent rate of conversion to open surgery despite the average tumor height being less than 6 cm from the anal verge.
A favorable study could shine an important spotlight on the transanal technique, while conveying good news to patients with rectal tumors encroaching on the sphincters for whom complete tumor response was not achievable through chemoradiation. Currently, many of these patients are offered no surgical option other than APR—a traumatic experience for many. Dr. Sylla laments this treatment shortfall, pointing to the existence of growing data showing that when done by well-trained surgeons at high-volume taTME centers, the approach results in high-quality resection of tumors close to the anal verge.

Patricia Sylla, MD, is the new Chief of the Division of Colorectal Surgery.
In her new role as System Chief of Colorectal Surgery, Dr. Sylla will continue to train surgeons and build strong collaborations with oncology practices and cancer centers to increase awareness of this surgical technique, especially for young patients with early-onset rectal cancer who are desperate to avoid a permanent stoma. “One of my greatest joys is to train the next generation of surgeons who are committed to mastering this approach,” she says.
One such surgeon is Sue Hahn, MD, Assistant Professor of Colon and Rectal Surgery at Icahn Mount Sinai, who has followed what Dr. Sylla considers an ideal training pathway. She first assisted Dr. Sylla as a surgery resident, then completed a one-year colorectal fellowship at UMass Chan Medical School, where she formally trained in taTME with an experienced group that had participated in the phase 2 taTME trial. Since returning to Mount Sinai two years ago as faculty, Dr. Hahn has further mastered the approach and is helping to grow the taTME program.
With her new platform, Dr. Sylla also intends to expand the division’s collaborative research capability. “Being able to offer cutting-edge procedures to patients through new clinical trials is a dream come true for me,” she says. “My mission is to bring together resources that now are scattered across the system to increase collaborations among specialists, and thereby grow the research enterprise in a way that hasn’t been done in the past.”
Featured

Patricia Sylla, MD
Professor of Surgery