Related Article
Pancreatic cancer—the third leading cause of cancer death in the United States—is typically thought of as a terminal diagnosis, even by professionals in the field. The five-year survival rate for pancreatic adenocarcinoma remains around 9 percent.
But the tide could well be turning thanks to advanced new treatments and aggressive surveillance. Indeed, recent studies have underscored the benefit of high-risk pancreatic surveillance programs that have helped push the three-year survival rates as high as 85 percent in some cases, in large part by catching a higher proportion of malignant lesions while they are still resectable.
From the opening of its specialized pancreatic cancer surveillance program 10 years ago, Mount Sinai has been in the vanguard of the field. The focus is on early detection through active risk assessment—particularly in families where two or more immediate members have a history of the disease—led by a team of clinicians experienced in gastrointestinal cancers, working closely with genetic counselors. Tethered to this program is a robust research initiative driven by a registry of more than 800 high-risk patients who, in many cases, have undergone surveillance and agreed to participate in clinical trials.
“In our program, patients are offered a full risk assessment based on a very detailed three-generation family history focused on pancreatic cancer, as well as other neoplasms such as breast, ovarian, skin, and colon cancers,” says Aimee Lucas, MD, MS, Professor of Medicine (Gastroenterology) at the Icahn School of Medicine at Mount Sinai, who launched the surveillance clinic in 2012. “After seeing our genetic counselors, patients typically meet with me to plan a personalized clinical surveillance program, which may include endoscopic ultrasound or MRI. At the end of the visit, we draw blood for genetic testing and any clinical or research labs that might be indicated.”
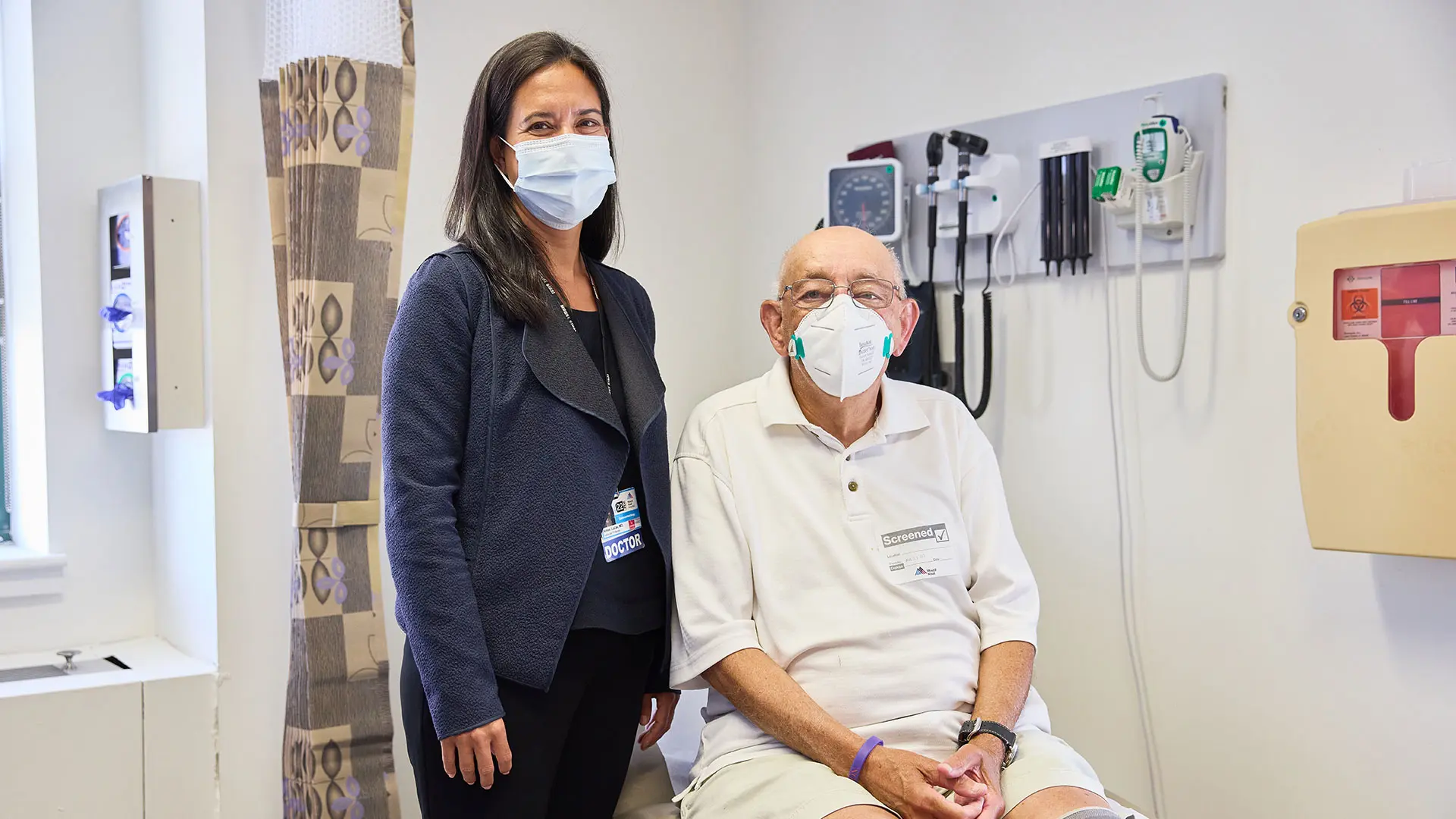
Aimee Lucas, MD, MS, has launched a pancreatic screening program for high-risk patients like Martin Abrams.
About a third of patients screened at the Upper East Side clinic in Manhattan show small, sub-centimeter pancreatic cysts on imaging. “The majority of cysts do nothing over time, so we simply watch them,” Dr. Lucas says. Some features, however, can serve as markers for neoplastic progression to high-grade dysplasia or pancreatic cancer, including the presence of multifocal cysts, cyst growth, or solid nodules.
In fact, telltale biomarkers are at the heart of Dr. Lucas’s growing body of research for detecting early pancreatic cancer. One study in which she was senior author found, for example, that high-risk patients with elevated hemoglobin A1c (HbA1c) were more likely to have pancreatic cysts compared to patients with lower levels observable through screening—findings that could be helpful in tailoring surveillance protocols for individuals at increased risk of developing pancreatic adenocarcinoma. Past research in the field has established new-onset diabetes mellitus as a precursor to pancreatic cancer, with approximately 85 percent of patients diagnosed with the malignancy also having impaired fasting blood glucose or diabetes.
In another study, Dr. Lucas significantly expanded the boundaries of that knowledge with the discovery that metabolic changes such as worsening glycemic control and weight loss may be harbingers of underlying pancreatic cancer. More specifically, she and her research team learned that glycemic elevations may occur up to three years before diagnosis, and weight loss up to two years prior to diagnosis. For that reason, they recommended including markers of glucose intolerance and body mass index trends in predictive models of pancreatic cancer.
“One of the major reasons pancreatic cancer remains so deadly is because of late detection,” Dr. Lucas points out. “That’s why we’re so focused on investigating genetic predisposition and biomarkers for early detection, and pairing that information with an aggressive surveillance program that could lead to improved outcomes.”
Featured Faculty and Division Leadership

Aimee Lucas, MD, MS
Professor of Medicine (Gastroenterology)

Bruce E. Sands, MD, MS
Dr. Burrill B. Crohn Professor of Medicine; Chief, Dr. Henry D. Janowitz Division of Gastroenterology
