Mount Sinai has burnished its reputation as a leading inflammatory bowel disease (IBD) center by deploying one of the nation’s first intestinal ultrasound machines for fast, accurate, and noninvasive assessment of ulcerative colitis (UC) and Crohn’s disease. The advanced procedure presages a new era for IBD patients who now have a way to visualize with their physicians during clinic visits the progress of their treatment, and whether changes are necessary.
“Intestinal ultrasound takes the guesswork out of decision-making for physicians and eliminates the need for expensive MRI and CT imaging and invasive testing like a colonoscopy,” says Marla Dubinsky, MD, Professor of Pediatrics, and Medicine (Gastroenterology), Icahn School of Medicine at Mount Sinai. “For patients, it’s a riskless and simple procedure that gives them the information they need on the spot to feel confident that their IBD is under control.”
Dr. Dubinsky was first introduced to intestinal ultrasound more than two decades ago as a gastroenterology fellow in Canada. Aware of its vast clinical and cost-savings potential for IBD, she was successful years later in bringing the technology to Mount Sinai with philanthropic support. While intestinal ultrasound has become the standard of care in Canada and many parts of Europe, it never gained a foothold in the United States, until now.
“Once patients have left an office visit with ultrasound, they can’t imagine going back to the traditional method of disease monitoring,” says Michael Dolinger, MD, a gastroenterology fellow at Icahn Mount Sinai whom Dr. Dubinsky recently sent to Europe for training in the technique. In September 2022, he will lead the country’s first training course for intestinal ultrasound in partnership with the International Bowel Ultrasound Group at Mount Sinai.
“The procedure provides incredible value to patients in the course of a 10-minute visit,” explains Dr. Dolinger. “We’re the only center of excellence in the United States that has fully integrated intestinal ultrasound into practice, and it’s exciting to know we’re leading the way for a field that’s on the verge of really taking off.”
“Once patients have left an office visit with ultrasound, they can’t imagine going back to the traditional method of disease monitoring.”
- Michael Dolinger, MD
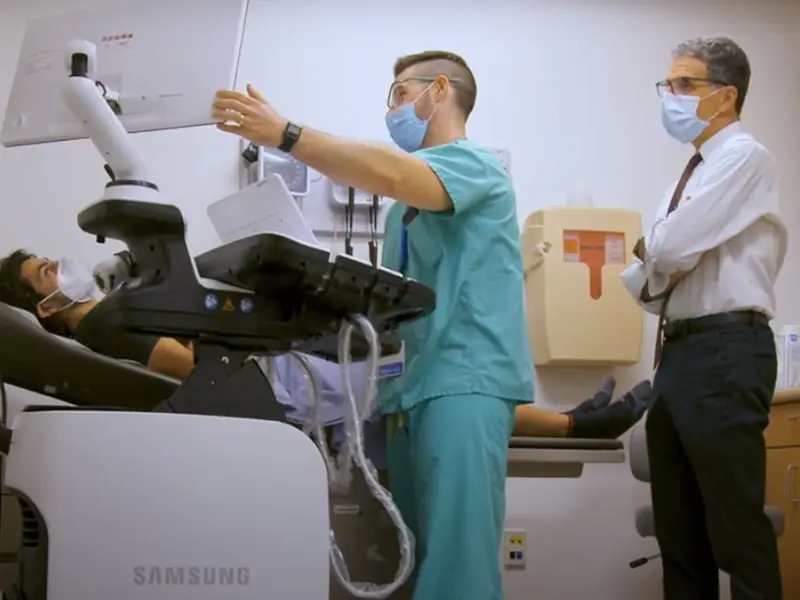
Michael Dolinger, MD, performs intestinal ultrasound on inflammatory bowel disease patient Evan Woods as the patient’s gastroenterologist, Keith Benkov, MD, observes.
As part of its groundbreaking work, the Division of Gastroenterology is actively involved in research and building a robust database of outcomes. Drs. Dubinsky and Dolinger, for example, recently authored a study published in Clinical Gastroenterology that found small bowel ultrasound to be a valuable, safe, and cost-effective modality to assess transmural healing in pediatric Crohn’s disease patients on infliximab therapy.
Over the past 15 months, Mount Sinai’s comprehensive Susan and Leonard Feinstein Inflammatory Bowel Disease Clinical Center has used ultrasound with more than 1,500 patients. Among the modality’s many benefits is the fact that patients are not required to prepare by fasting and drinking contrast. What’s more, intestinal ultrasound delivers extremely accurate results and can be repeated as often as the gastroenterologist wishes with no radiation exposure. It can also serve as a critical decision-making tool for IBD patients who are pregnant and can’t undergo invasive procedures, or those who have had a colectomy with a J-pouch and new ileum.
Powering the procedure is a high-definition machine from Samsung (the RS85 Prestige) that is more advanced than traditional ultrasound, permitting shear wave elastography with high-quality images that can highlight any scar tissue or chronic damage to the bowel. “It’s especially helpful when you can show patients in real time their disease activity, improvement, or remission,” says Dr. Dolinger. “And it can be convincing for parents who are faced with the decision of starting a child on lifelong immune therapy.”
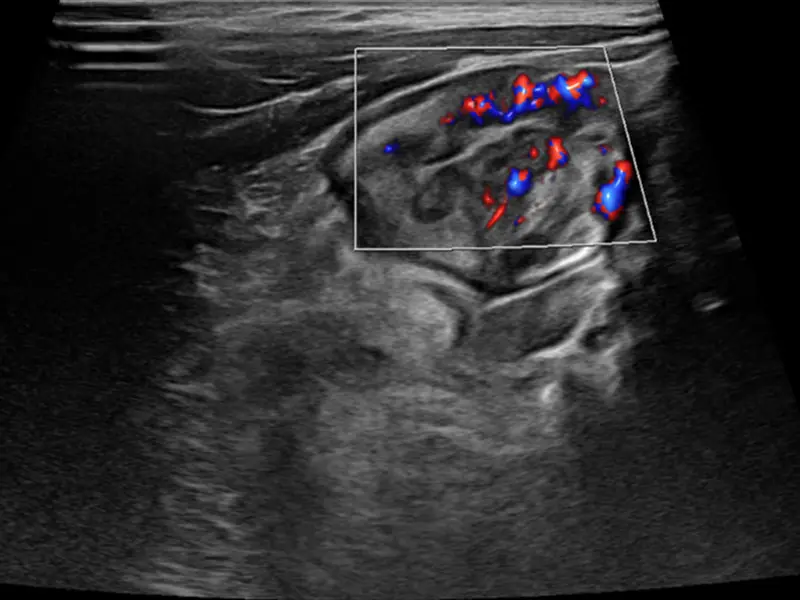
The end of the small bowel called the terminal ileum, which is inflamed in a 7-year-old boy before he begins a new therapy for his Crohn’s disease.
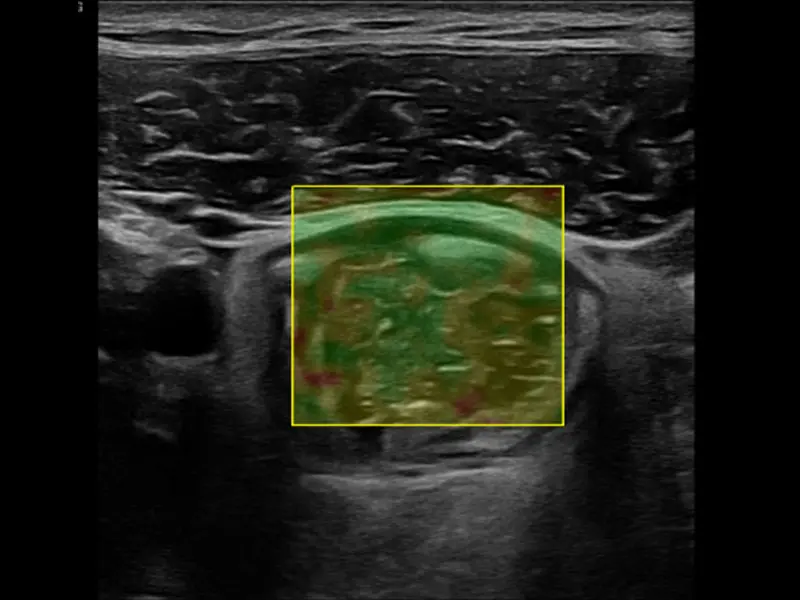
A shear wave elastography—how we measure scar tissue in the small intestine.
Looking back on her own years-long infatuation and tireless work with intestinal ultrasound, Dr. Dubinsky couldn’t be more pleased to see it finally emerge as a vital clinical tool for patients and physicians at Mount Sinai. “I realized there was no reason in light of our reputation and the volume of our IBD Center that we shouldn’t be leading this transformation,” she declares. “There’s an urgency to make sure no patient is left behind.”
Featured

Michael Dolinger, MD
Gastroenterology fellow, Icahn School of Medicine at Mount Sinai

Marla Dubinsky, MD
Professor of Pediatrics (Pediatric Gastroenterology)