A new Mount Sinai study is investigating the pathophysiological, prognostic, and surgical potential of 7-Tesla magnetic resonance imaging (MRI)—the most powerful imaging technology available—among patients who present with acoustic neuromas.
“The ability to visualize the relationship of the tumor to the cochlear nerve and to the seventh cranial nerve in the internal auditory canal is very important for us,” says George Wanna, MD, Chair of Otolaryngology at New York Eye and Ear Infirmary of Mount Sinai and Mount Sinai Beth Israel, and Executive Vice Chair of Otolaryngology at the Mount Sinai Health System.
The study is recruiting 20 participants with acoustic neuromas who have not previously undergone surgery, and who do not have a metal cranial implant. The research team will assess the technology’s ability to visualize factors such as anatomy, vascularity, location of the cranial nerves, the secondary audio pathway, and the tumor itself.
“It will enable us to preserve hearing and achieve better facial outcomes among patients who present with these tumors in collaboration with neurosurgery,” explains Dr. Wanna, who is also Professor of Otolaryngology, and Neurosurgery, at the Icahn School of Medicine at Mount Sinai. “It will also give us a better understanding of the relationship between the tumor and the structure of the ear, which will enable us to tailor the surgery to achieve the best possible outcome for the patient.”
The first time Raj Shrivastava, MD, used the 7-Tesla MRI for anatomic visualization of cranial nerves among patients with pituitary adenomas, he was impressed. In fact, the degree of detail he observed exceeded his expectations.
“It was remarkable,” says Dr. Shrivastava, Professor of Neurosurgery, and Otolaryngology, at Icahn Mount Sinai, and Vice Chair of Education for the Department of Neurosurgery at the Mount Sinai Health System.
“We were able to see the nerves running through the tumor, the blood vessels, even distal projection connectivity with such clarity that we can anatomically map those connections in a way that was not possible before. We also observed anatomic changes to the cortex resulting from the tumor, which was unexpected but fascinating.”
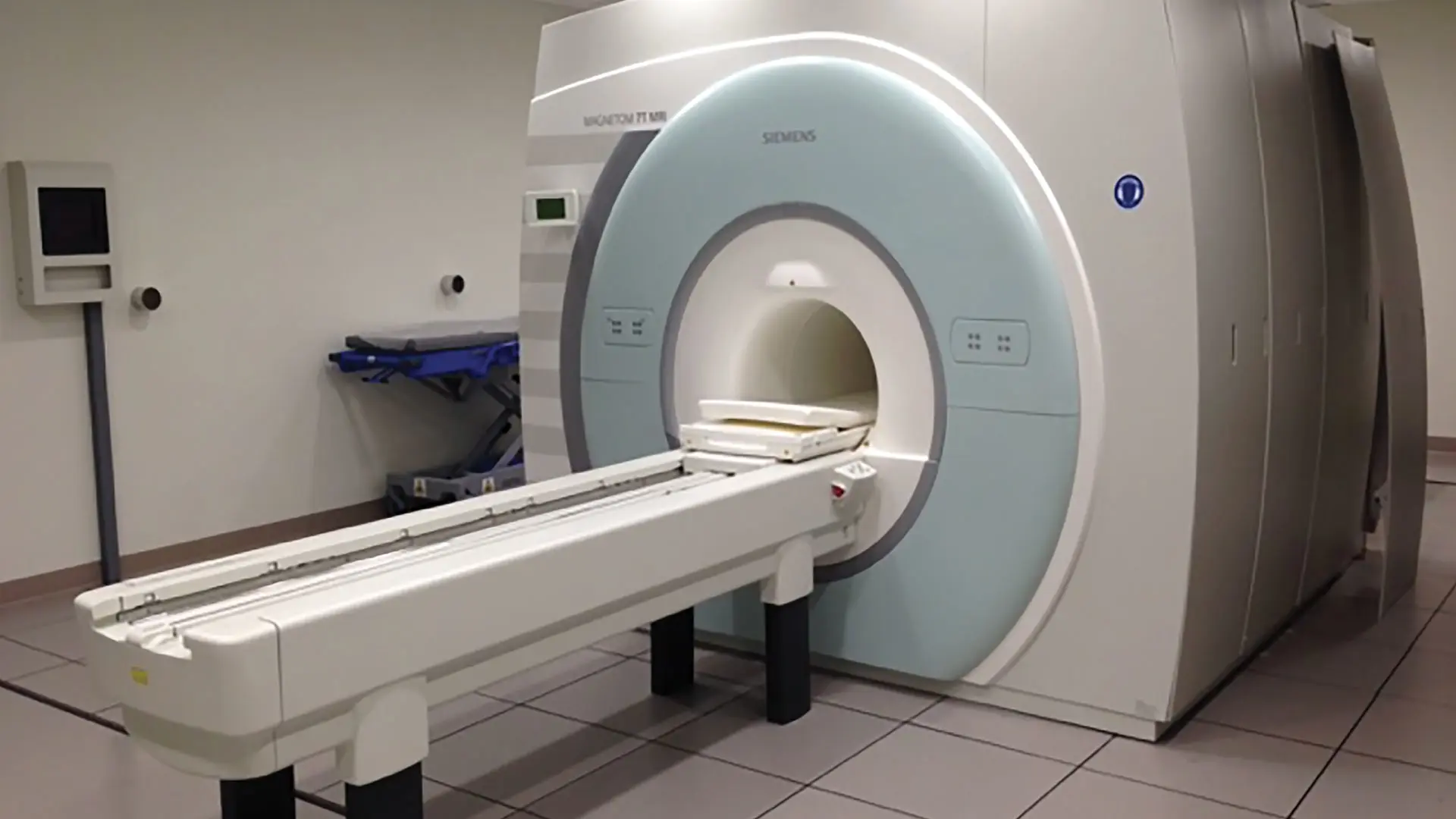
7-Tesla MRI.
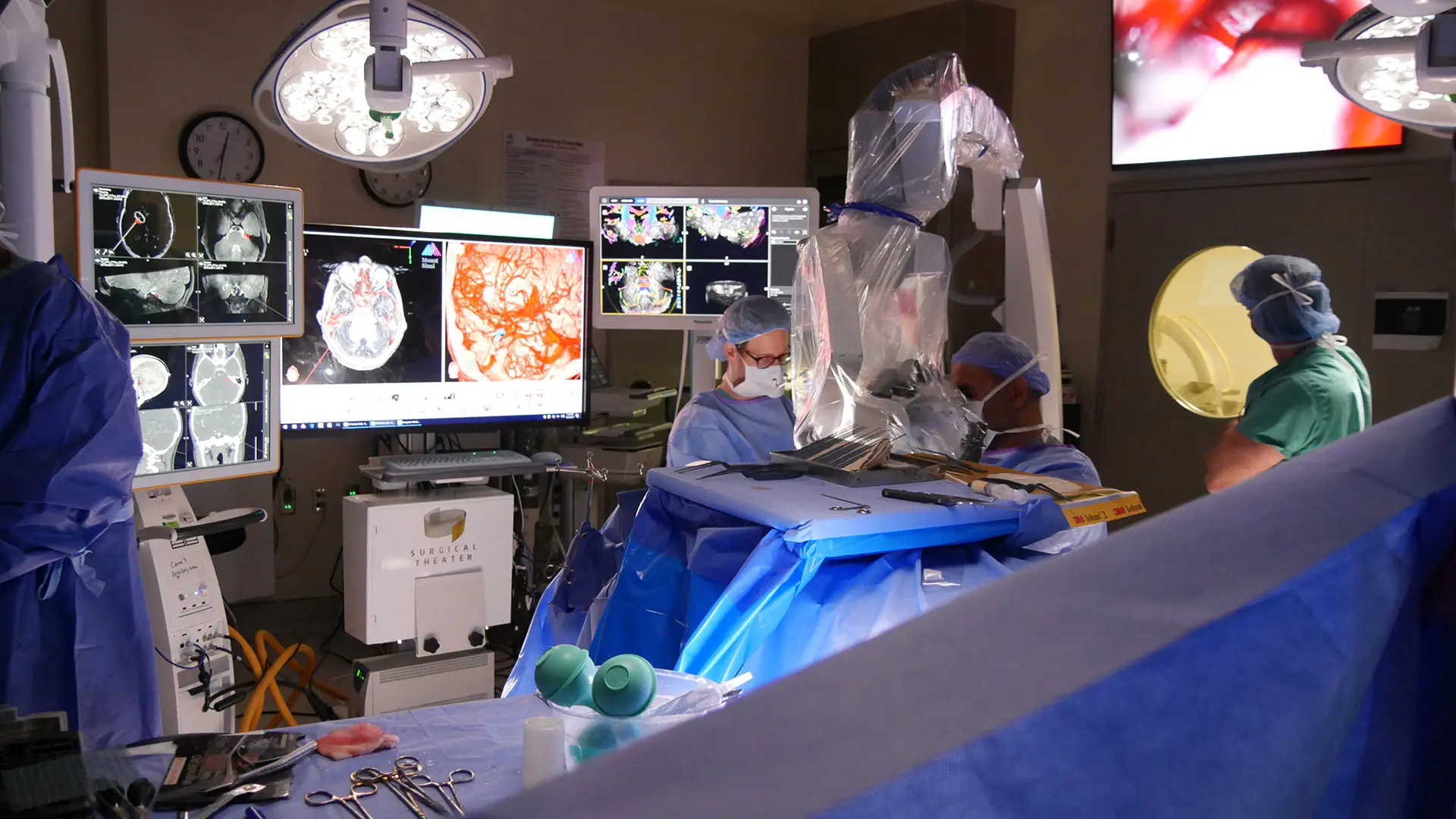
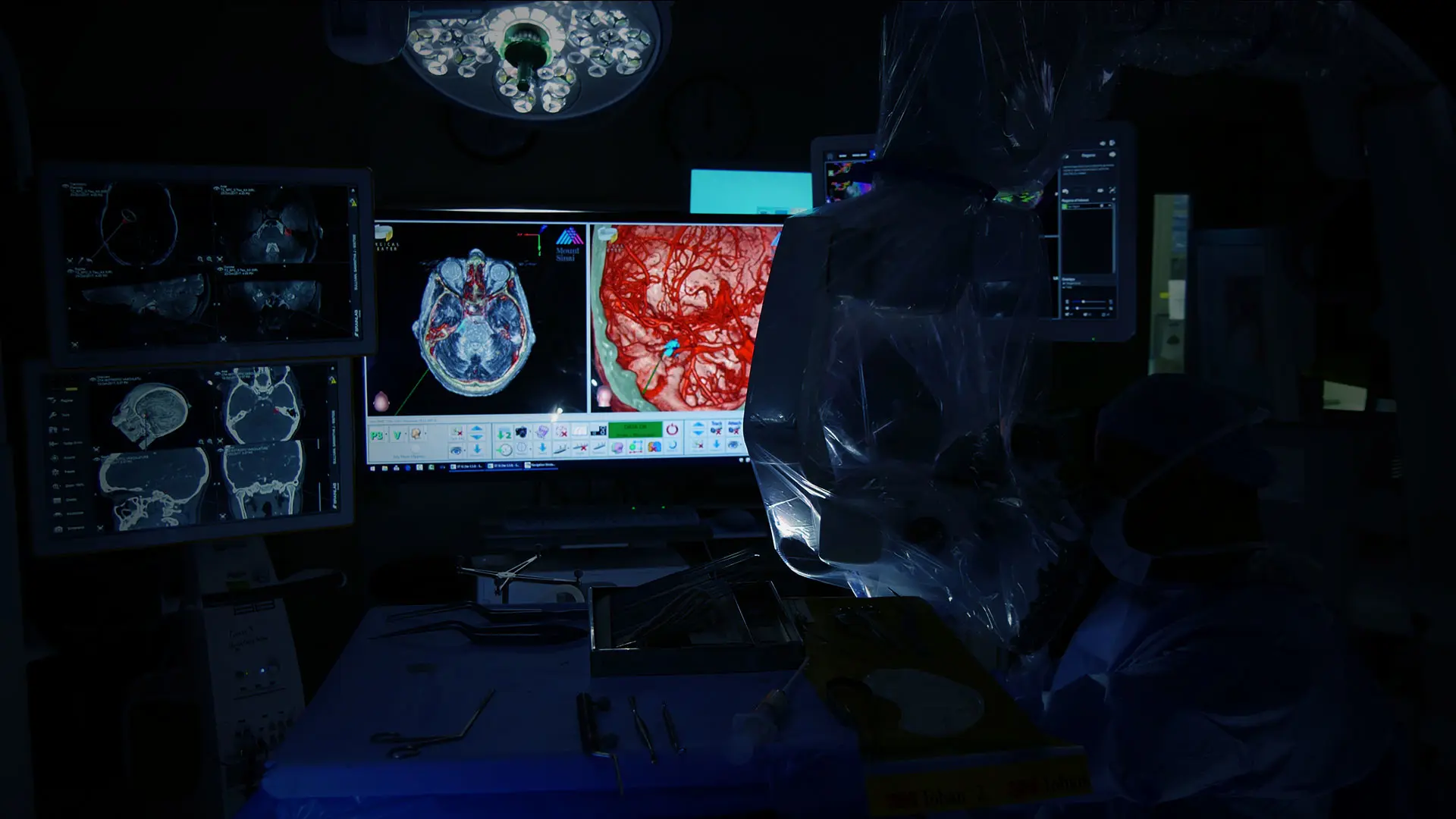
Anatomic visualization of cranial nerves from 7-Tesla MRI in the operating room.
How the 7-Tesla MRI Could Lead to Better Patient Outcomes
If successful, the study could establish the 7-Tesla MRI as a more effective tool than facial nerve stimulators in minimizing the risk of treatment-related complications, such as facial nerve paralysis, loss of hearing, and tumor bleeding among patients who present with acoustic neuromas. But Dr. Wanna is already thinking about other otolaryngological applications of the technology, such as investigating potential anatomical factors associated with hearing loss or Meniere’s disease, that would be beneficial for patients.
“Right now, we are only able to definitively diagnose Meniere’s disease postmortem,” Dr. Wanna says. “If the higher resolution of this technology is able to deliver new insights on the disease etiology, we could potentially diagnose it immediately or even identify new therapeutic targets.”
The study also holds the potential to advance understanding of the downstream impacts of acoustic neuromas on the cochlear nerve, and thus help set patient expectations for both the length and degree of postoperative recovery. In a study of the technology involving lesions of the skull base, a research team led by Priti Balchandani, PhD, investigated imaging metrics that displayed or indicated damage to cranial structures due to the presence of the lesion—something that had not been thoroughly explored previously.
“In addition to providing a better visualization of the main anatomy often involved in surgical decision-making, the 7-Tesla MRI technology also enhanced our understanding of the pathophysiology of the disease and its effects on both the brain and brain function, and that enabled us to link those effects to prognosis,” says Dr. Balchandani, Professor of Diagnostic, Molecular, and Interventional Radiology, Neuroscience, and Psychiatry; Director of the Advanced Neuroimaging Research Program; and Associate Director of the BioMedical Engineering and Imaging Institute, all at Icahn Mount Sinai.
The study has resulted in several publications, including a paper, published in the Journal of Neurological Surgery Part B: Skull Base, reporting the overall utility of the 7-Tesla MRI for surgical resection of pituitary adenomas. “Based on those findings, we believe the acoustic neuromas study will demonstrate that 7-Tesla MRI is invaluable in both the treatment and prognosis of these lesions,” Dr. Balchandani says.
Looking Beyond Acoustic Neuromas
Although the acoustic neuromas study is in its early stages, Mount Sinai researchers are preparing a one-year National Institutes of Health-funded research project to explore the potential of 7-Tesla MRI to determine disease etiology among patients who present with trigeminal neuralgia. There are also plans for a pilot study of the technology’s efficacy in guiding radiation therapy dosage decisions among patients who have malignant lesions of the skull base. The imaging collected through these and other initiatives will form the basis for a database that could support the development of a predictive algorithm for various otolaryngological conditions.
“We have to ask the right questions to build the algorithm, but we need more data from the 7-Tesla MRI to make that possible,” Dr. Wanna says. “I expect that in the next five years, we may be able to build something really meaningful.”
Featured

George Wanna, MD
Professor of Otolaryngology and Neurosurgery

Priti Balchandani, PhD
Professor of Diagnostic, Molecular, and Interventional Radiology, Neuroscience, and Psychiatry

Raj Shrivastava, MD
Professor of Neurosurgery and Otolaryngology