In the safe clinical environment of New York Eye and Ear Infirmary of Mount Sinai, patients undergoing standard-of-care therapy for vestibular dysfunction typically demonstrate progress in their gait and balance. But those gains are hard to maintain when navigating the streets of New York City.
“Uneven sidewalks, ramps, traffic noise, and crowds pose considerable balance and stimuli challenges for our patients,” says Jennifer Kelly, PT, DPT, NCS, Supervisor of Rehabilitation Services at the Ear Institute and Assistant Professor of Otolaryngology at the Icahn School of Medicine at Mount Sinai. “We found that they were still experiencing symptoms during these high-level activities that are hard to replicate in the clinic. Based on that feedback, we started thinking about how we could create a bridge for patients to confidently navigate those real environments.”
Virtual Reality Can Help Patients Learn at Their Own Pace
The Vestibular Rehabilitation team at Icahn Mount Sinai, led by Dr. Kelly, partnered with the physical therapy, music science, and computer science departments at the New York University (NYU) Steinhardt School of Culture, Education, and Human Development to develop a prototype virtual reality (VR) system for therapeutic interventions among patients with vestibular dysfunctions. Using HTC VIVE VR headsets, patients are trained to navigate either an abstract or a busy environment that has been customized to address their specific vestibular dysfunction challenges. Dr. Kelly believes that this context-based training approach to VR therapy distinguishes this prototype from other systems, which have adopted a game-based approach.
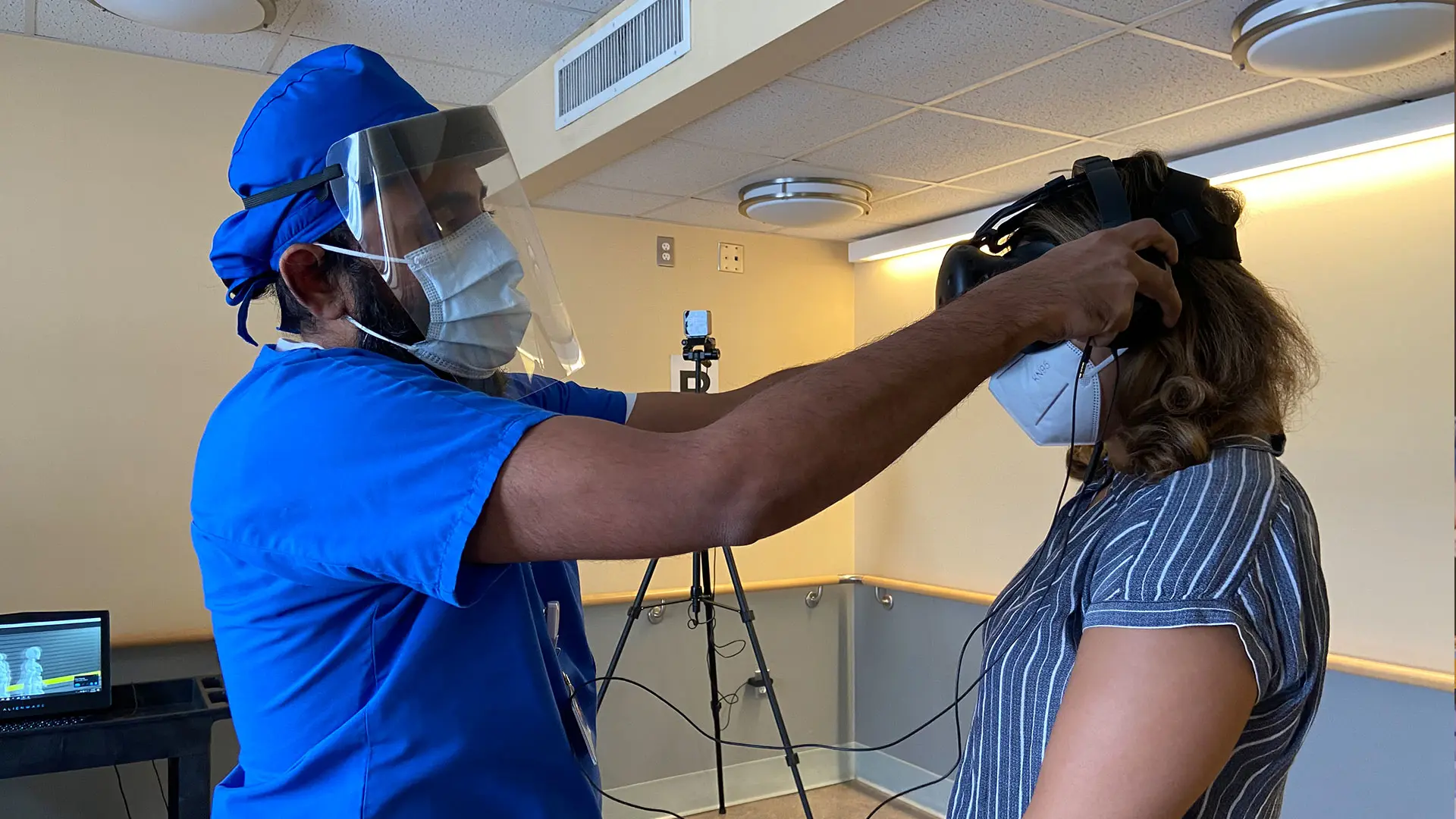
A patient (right) is fitted with a VR headset.
“For example, for the busy environment, they have a choice of a city street, subway, airport, or park scenario,” Dr. Kelly explains. “We consult with the patient about these options and where they would like to start. It is a graded experience, so we can adjust elements such as their direction, their speed, the number of people around them, and stimuli such as signage and sound to approximate a real-life experience.”
There are some limitations to the realism that the system delivers. For one, the VR experience is delivered in a space that has a walking span of four feet. Furthermore, the scenarios are not hyperrealistic. But these limits are believed to be beneficial for patients, resulting in a controlled environment that mitigates the stress associated with navigating real-life situations.
“Visual movement is a significant trigger for our patients’ symptoms,” Dr. Kelly says. “We do not want to overwhelm them. For that reason, the people who approach them in the simulation do not look like real people, which helps to reduce their stress levels, as does the ability to offer a graded experience so we are not starting them off with something that approximates rush-hour chaos. Essentially, we are creating an opportunity for them to engage in an environment they might normally avoid and do so without the anxiety that would make it difficult to learn from and adapt to these scenarios. That has the potential to keep them moving and socializing and thus avoid a downward physical and mental spiral.”
Advancing the Prototype With a Pilot Study
Based on these factors, Dr. Kelly and the team believe this prototype system would result in improved outcome measures versus traditional vestibular rehab—a hypothesis she explored through a pilot study. The goal was to recruit 28 patients and randomize them on a one-to-one basis into VR and standard treatment cohorts, both of which would also engage in-home exercise programs. However, the COVID-19 pandemic limited recruitment to 18 participants—10 who underwent VR treatment and eight who underwent standard treatment.
Using traditional outcome measures, such as functional gait, dizziness, confidence scale, and the visual vertigo analog scale, Dr. Kelly found that both cohorts achieved similar results. “That was surprising,” she says. “Does that mean home exercise was the most important element, or is movement the most important factor regardless of approach? Those are questions we need to explore further. The main takeaway is that everyone demonstrated improvements in fall risk and subjective scores across the board.”
Regardless, some patients in the VR treatment cohort indicated that this approach was more tailored to their functional challenges than traditional forms of therapy—another reason it merits further study. Dr. Kelly and the research team at Mount Sinai and NYU are interested in conducting multisite studies to gain more insights on the efficacy of the prototype. She is also interested in assessing the impact of VR therapy among patients who have experienced a concussion. But she has a more ambitious plan in mind for this technology.
“Although we are fortunate to be in an urban environment where people have access to vestibular dysfunction programs and experts, those resources are not as accessible for patients across the country or around the world,” Dr. Kelly says. “For that reason, we are interested in seeing whether it is possible to bring this therapeutic modality safely into patients’ homes. Our collaborators in computer science at NYU are working to realize that goal.”
Featured

Jennifer Kelly, PT, DPT, NCS
Assistant Professor of Otolaryngology