It took some time for Satish Govindaraj, MD, to fully embrace balloon sinuplasty as a treatment for sinusitis patients. It was not the procedure itself that concerned him; it was the fact that he had to rely on transillumination to perform it.
“Sometimes, if the target sinus is really diseased or small, the light is not sufficient to know if you are truly in the sinus or not,” says Dr. Govindaraj, Chief of the Division of Rhinology, and
Vice Chair of Clinical Affairs in the Department of Otolaryngology-Head and Neck Surgery at Mount Sinai. “From a safety standpoint and from a confirmation standpoint, it did not provide the certainty I wanted.”
This commitment to patient safety prompted Mount Sinai’s Department of Otolaryngology-Head and Neck Surgery to become the first academic center in New York City to adopt ENT
Navigation balloon sinuplasty. This cutting-edge tool delivers innovative features such as automatic merging of the patient’s CT and MRI scans, as well as real-time confirmation to enhance the ability of ear, nose, and throat surgeons to perform minimally invasive procedures in-office for sinusitis patients.
“When you incorporate navigation technology into the procedure, everything is easily defined. We are able to divert patients from undergoing surgery under general anesthesia in the operating room, which means a quicker recovery,” says Dr. Govindaraj, Associate Professor of Otolaryngology-Head and Neck Surgery at the Icahn School of Medicine at
Mount Sinai. “I typically perform the procedure on Friday and by the next day—or Monday at the latest—the patient is back to normal activity.”
Before undergoing the procedure, patients are assessed to ensure they are amenable to balloon-based sinuplasty and that the disease involves the frontal, maxillary, or spheroid sinus. Once the affected sinus cavity is completely anesthetized, Dr. Govindaraj places a sensor on the patient’s forehead, traces points on their face, and those points are linked to
the patient’s CT scan, which is entered into the navigation system. This enables Dr. Govindaraj to see the location of the guidewire tip on the patient’s CT scan, resulting in real-time confirmation that he is following the correct tract into the target sinus. After dilating the sinus, Dr. Govindaraj is able to take cultures and use the balloon tip to irrigate and flush the sinus, effectively clearing it of any mucus or bacteria.
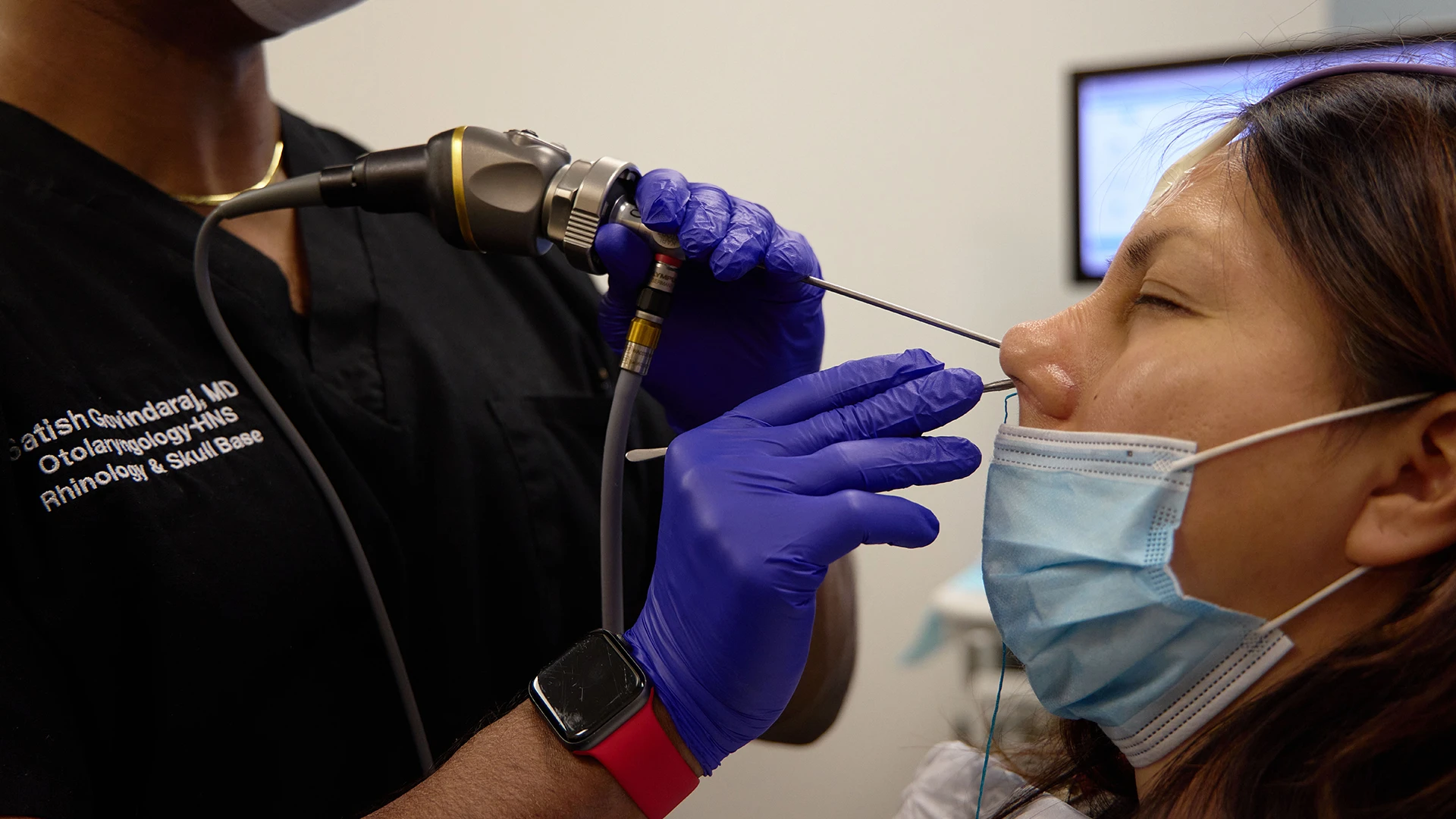
Local anesthesia is applied to the nose and sinus cavity to ensure a pain free experience.

Using image-guided CT scans, surgeons can precisely navigate through the nasal passageways to the target sinus.
“One of the risks in sinus surgery is communicating with the brain area as well as the eye area,” Dr. Govindaraj says. “The guidewire is very soft, so the risk of complication is low with balloon sinuplasty, but the ability to see where the guidewire is going lowers that risk further. It is safer, more efficient, and it enables you to navigate complex anatomy in order to reach and dilate the true sinus without creating an alternate opening.”
To date, Dr. Govindaraj and his team of rhinologists have performed balloon sinuplasty with ENT navigation numerous times and have consistently achieved positive outcomes. “We track our pre- and post-procedure outcomes with a validated quality-of-life questionnaire appropriately called the SNOT-22.” He mainly offers the procedure to patients with acute or chronic sinusitis, but he also performs balloon sinuplasty among patients who present with stenosis of the sinuses following surgery. “Sometimes if the stenosis recurs, we may have to re-dilate the sinus,” he explains. “But it is very uncommon to redo the procedure among patients with acute or chronic sinusitis. They may become infected again, but our goal is to reduce the frequency, severity, and the acute symptoms.”
Dr. Govindaraj anticipates that continued evolution of ENT navigation technology will enable him to perform the majority of his surgical procedures for acute and chronic sinusitis in the office setting.
“Patients want a quicker recovery and less inconvenience to their daily life. The office offers them that option,” he says. But just like with any surgical procedure, patient selection is critical to success in the office. To assess this, Dr. Govindaraj and his team have an open dialogue with patients to select the appropriate setting based on their level of disease and medical history.
“Bringing operating room technology into the office setting is the future of sinus and polyp treatment,” he says. “We are now doing these cases across the Health System. I am pleased that our rhinologists can offer this treatment option to our patients. As an academic center we need to be leaders in this treatment modality and provide patients with the state-of-the-art care they deserve.”
Featured

Satish Govindaraj, MD
Associate Professor Otolaryngology-Head and Neck Surgery