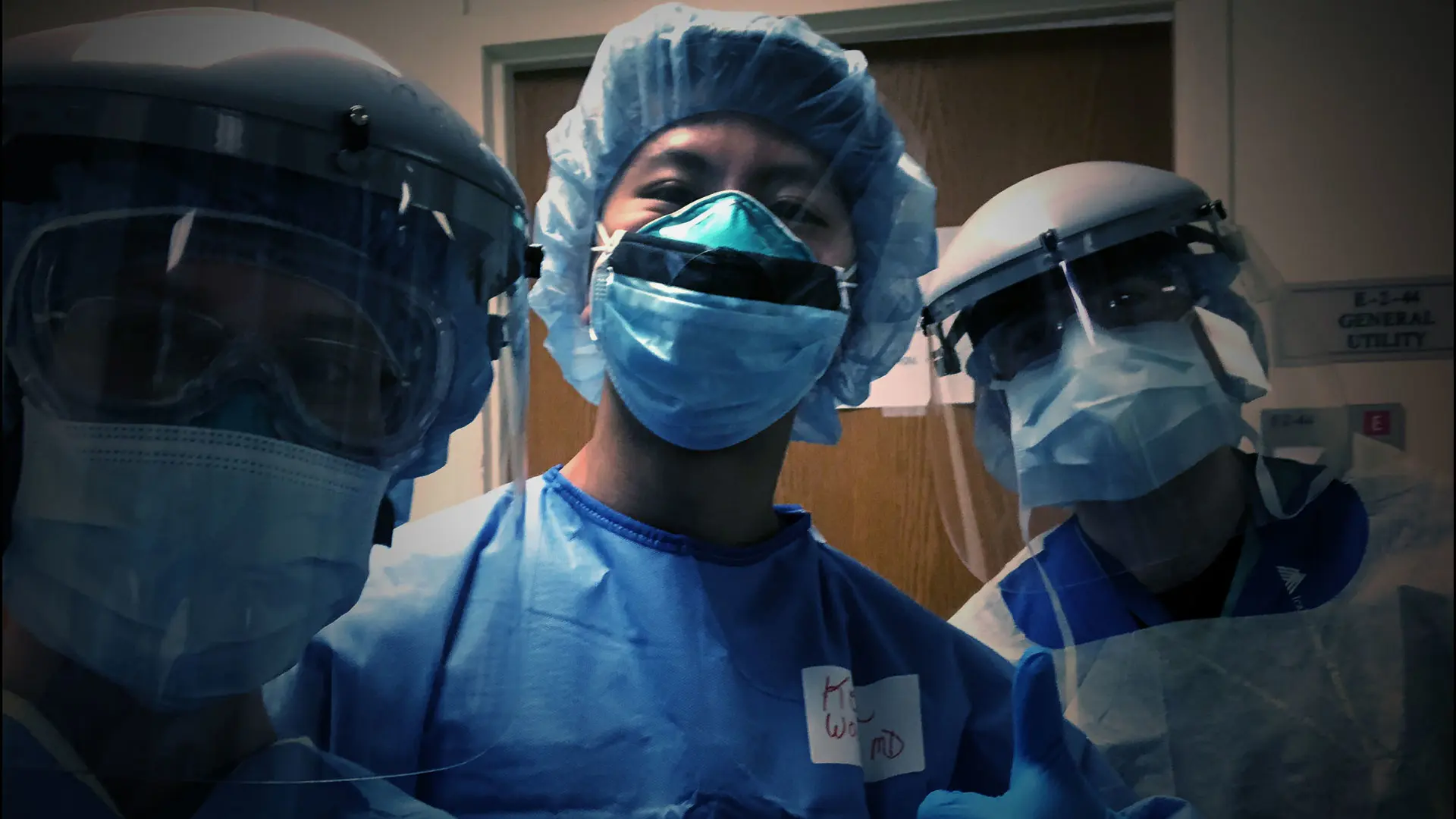
In the spring of 2020, COVID-19 anxiety was on the rise at Elmhurst Hospital Center, a Mount Sinai Health System affiliate in the New York City borough of Queens. In response to increased cases of the novel coronavirus, the Department of Otolaryngology - Head and Neck Surgery at Mount Sinai had halted all nonurgent and elective cases and transferred the majority of appointments to telehealth. Throughout the hospital, medical wards were converted to COVID-19 intensive care units (ICUs) and the number of patients intubated threatened to overwhelm resources. Though the initial thinking was to keep residents away from the front lines and safe from infection, reinforcements were desperately needed and residents were eager to assist in the effort.
Launched in March 2020, the seven-bed unit distinguished itself as the nation’s first ENT/Otolaryngology-run COVID-19 ICU. Members included Arvind Badhey, MD; Benjamin Laitman, MD, PhD; Usmaan Basharat, MD; Jaclyn Klimczak, MD; Eliezer Kinberg, MD; Kevin Wong, MD; Peter Filip, MD; Caleb Fan, MD; Douglas Worrall, MD; Noel Phan, MD; Christine Barron, MD; and substitutes Joshua Zeiger, MD; Shirley Hu, MD; and Andrey Filimonov, MD. The group was organized into four teams of three residents, all of whom received guidance from attending physicians in Critical Care and additional support from ENT attending physicians.
Strategizing in the Face of Uncertainty
“I did not want us to rush in, start this up, and see how it goes,” says Dr. Klimczak of the COVID-19 unit. “We needed to step back and formulate a strategy so that we not only achieved positive outcomes for our patients but also protected ourselves from infection.”
The unit was committed to careful planning that addressed uncertainty about the virus and its impacts. Part of the strategy involved residents sourcing personal protective equipment, researching best practices for delivering ICU care, and consulting with physicians in Italy and China on their pandemic experiences.
It was invaluable preparation, but fears remained. “I have a wife and daughter and I did not want to bring this infection home with me,” Dr. Laitman says. Additionally, there were concerns that residents were not fully trained to take on an emergency of this magnitude, but the ability of the group—coupled with the critical need for skilled medical professionals—quelled apprehension. “We quickly came to grips with the fact that every single health care worker was needed in this battle and that, by stepping up, we could make a difference.”
For the most part, anxieties about the virus began to dissipate once residents began working in the unit and saw how many people were fighting for their lives. But there were still logistical challenges to contend with as residents contended with a novel virus. This includes determining appropriate ventilator settings and obtaining thoracic imaging, lab results, and dialysis referrals for COVID-19 patients who developed acute kidney injury. The many unknowns forced residents out of their comfort zones, but Dr. Kinberg believes the chaos served to bring out the best in everybody.
“We may not be intensivists, but we know the fundamentals for running a unit, we have experience in addressing respiratory distress, and we all know each other personally,” says Dr. Kinberg, who believes that a combination of knowledge and mutual trust made the residents a strong, stable team. “There was a real spirit of collaboration that enabled our unit to run substantially smoother than any of us anticipated.”
A Band of Brothers and Sisters Anchored by a Strong Support System
For Dr. Klimczak, the biggest struggle was the sheer number of COVID-19-related deaths that occurred when the ICU was active. “I think it was probably one of the toughest experiences I ever had to go through. Up until that point, I had not been exposed to death during my residency,” she explains. “Our unit came up with coping mechanisms and rituals, such as clapping when patients came off a medication or a ventilator, and residents made a point of checking in on each other. That really helped to ease the trauma that we witnessed each day.”
For Dr. Laitman, blogging his experiences served as a balm after particularly rough days. It also provided an opportunity to remain connected and share information with family and friends during the height of the pandemic. “Sometimes, it was just too hard to talk about, so writing it out was better,” he says. “But, it is also something I can show my daughter one day so she knows what we went through. Maybe she will be proud of the work we did.”
Marita Teng, MD, Residency Program Director for the Department of Otolaryngology - Head and Neck Surgery, also regularly checked in with Dr. Badhey as a mentor and colleague. She and Diana Kirke, MD, a laryngologist and head and neck surgeon at The Mount Sinai Hospital, kept abreast of details, including when days became especially difficult. In an effort to build resilience, Dr. Kirke hosted a mental health seminar with the residents that evolved into a daily huddle.
“After we told her some of our stories, Dr. Kirke got emotional, and that opened the door for the rest of us to express ourselves,” recalls Dr. Badhey. “She is so respected in the field, so for her to say, ‘It’s okay; this is really awful,’ was very refreshing. She was open and willing to listen to us. Her empathy broke down the hierarchy and gave us a communication channel that was much needed.”
How the ICU Prepared Residents for the Future
Although the sounds of the low-oxygen sirens still ring through his mind as he walks the hallways of Elmhurst Hospital, Dr. Kinberg also recalls the success stories, such as the older patients who recovered, went home, and celebrated one more birthday with their families. “That gives you a real appreciation for the role of the hospital in the community,” he says. “Particularly a hospital like Elmhurst. You see the impact it had through the years, such as the early days of HIV, during the H1N1 virus, or responding to the World Trade Center attack on September 11, 2001. That inspires you to be an advocate and ensure that all patients have access to care.”
“I know more about intensive care than ever before and know how to better manage these critically ill patients,” remarks Dr. Badhey, who is now a head and neck microvascular fellow at the University of Cincinnati. The experience, Dr. Badhey believes, allowed him and his colleagues to have more intelligent conversations with anesthesiologists about patients. “We are swift critical decision-makers and more prepared for our future than we could have ever imagined.”
Dr. Klimczak agrees, adding that the pandemic reinforced the importance of making time for patients and their families. “We live in a very rushed society,” she says. “It is too easy to look at what we do as a job and forget that our patients have lives, families, perspectives, and hopes. COVID-19 was a reminder to always maintain humanity in treating patients, and the time you spend with them can make all the difference. Having gone through it, I think it has made us all better physicians.”
Featured
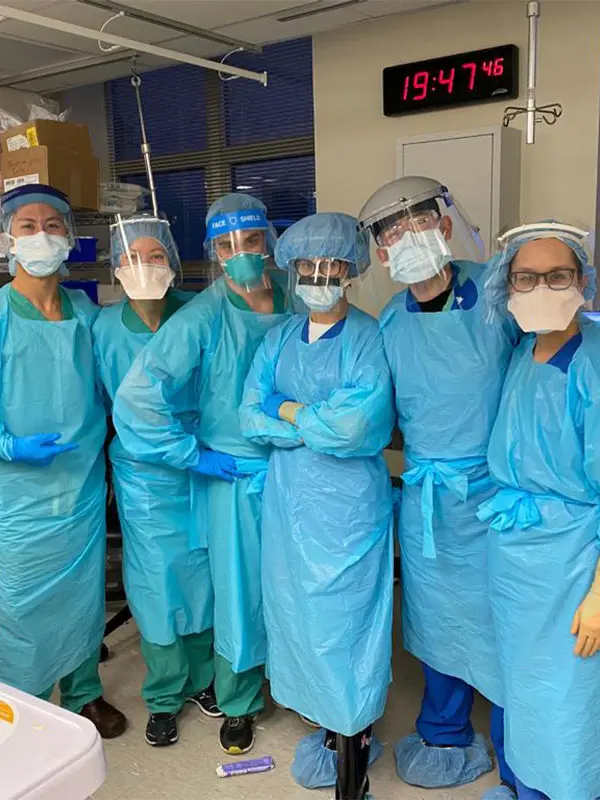
Otolaryngology - Head and Neck Surgery Residents
Icahn School of Medicine at Mount Sinai