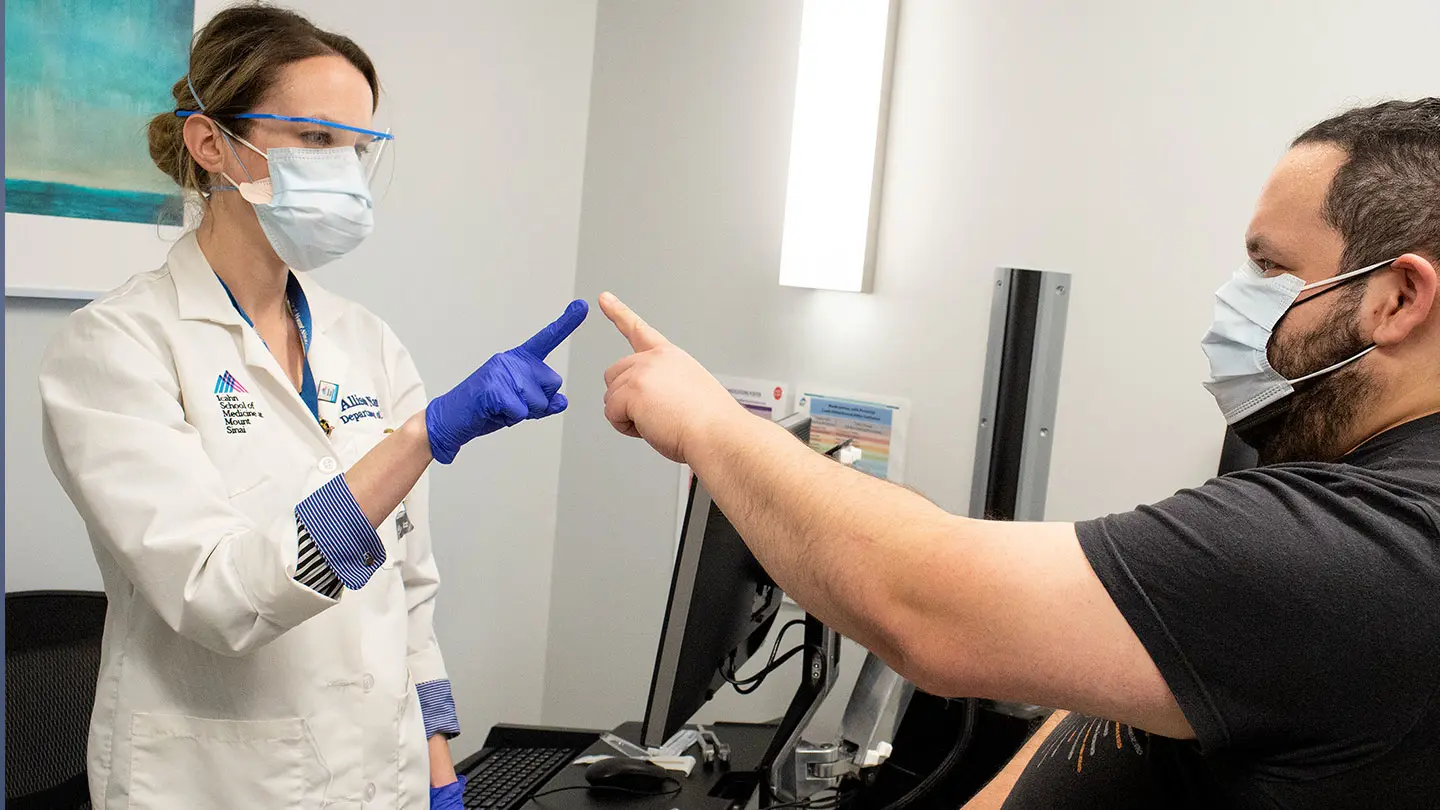
Long after the initial wave of COVID-19 cases in New York City had subsided, many patients were still experiencing damaging aftereffects. To help these still-vulnerable individuals, Mount Sinai Health System created the country’s first Center for Post-COVID Care (CPCC), which provides personalized, multispecialty care to recovering patients while gathering vital clinical data on a disease whose full effects are still not well understood.
“We saw the need, even while our caseloads were high, for a center that could provide comprehensive, expert care for a wide range of patients who continued to be impacted by this complex disease,” says Zijian Chen, MD, Assistant Professor of Medicine (Endocrinology, Diabetes, and Bone Disease) at the Icahn School of Medicine at Mount Sinai, and Medical Director of the Center for Post-COVID Care. “It was also important to us that all New Yorkers, regardless of their disease state or socioeconomic status, received that broad level of care from our team of medical specialists.”
An estimated 30 percent of COVID-19 survivors suffer from a variety of chronic conditions, Dr. Chen says, including increased risk of thromboembolic disease, cardiovascular complications, hepatic and renal impairment, and systemic inflammatory response syndrome. Moreover, patients who fought for their lives in hospital intensive care units may, months later, manifest mental health issues such as post-traumatic stress disorder, anxiety, and depression. As of January 2021, the Center had treated nearly 2,000 of these patients, sometimes called “long-haulers.”
Dr. Chen, who is also Medical Director of Mount Sinai Union Square, helped launch the Center for Post-COVID Care at the site in May 2020. And he still maintains his practice as an endocrinologist, treating patients with diabetes and a range of thyroid disorders.
Type 2 diabetes is among the most important risk factors for COVID-19. “Anybody with comorbid conditions is very susceptible to the infection itself,” Dr. Chen says, “but also susceptible to having more morbidity and mortality when they get infected with COVID.” Patients with type 2 diabetes are often also overweight, and according to the Centers for Disease Control and Prevention, the risk of severe illness from COVID-19 is higher for patients with a BMI of 30 or above. In addition, patients with COVID-19 are sometimes treated with steroids for inflammation—a poor option for patients with diabetes because it affects glucose control.
“We saw the need, even while our caseloads were high, for a center that could provide comprehensive, expert care for a wide range of patients who continued to be impacted by this complex disease.”
Zijian Chen, MD
The pandemic’s long periods of quarantine can lead to inactivity and overeating, which also are especially detrimental to patents with type 1 and type 2 diabetes. “For some patients, their glucose control was worse after the six months of seclusion,” Dr. Chen says, “not directly because of COVID but due to the circumstance that they are put in.” Conversely, some patients with diabetes are improving in the same situation. “You’re looking at patients who are homebound. They can’t go eat out whenever they want, and they can’t go to McDonald's to get French fries, or any other junk food,” he says. “So they’re actually losing weight, and their diabetes control is getting better."
The Center for Post-COVID Care is marshalling an array of advanced clinical tools and research expertise at Mount Sinai to evaluate the long-term systemic impact of COVID-19 on patients. This arsenal includes high-resolution CT imaging—a vast diagnostic improvement over the simple chest X-rays taken of patients presenting with upper airway symptoms and advanced respiratory distress in the early months of the viral outbreak. Once it opened, the Center also began offering pulmonary function tests to monitor lung performance. And it monitors the oxygen needs and other vital signs of recovering COVID-19 patients from their homes through Mount Sinai’s expanding telemedicine capability.
The linchpin of the Center’s investigative work, however, is its COVID-19 Registry, which collects baseline information of participating patients in varied areas such as comorbidities, socio-demographics, behaviors, mental health, and medications. Researchers further obtain baseline measures of pulmonary symptoms and physical indicators such as biometrics, spirometry, EKG, bloodwork, and antibody titers for SARS-CoV-2, the virus that causes COVID-19.
The registry’s goal is to inform further research and treatment around the world. The Center for Post-Covid Care is also advising institutions on setting up similar comprehensive care programs. At Mount Sinai, the Center is expected to expand to more sites throughout the Health System. But as a clinician, Dr. Chen has a completely different end-goal in mind.
“Ultimately, I hope the need will actually go away,” he says. “I say this because these post-COVID patients are suffering, and I’m hoping that through clinical care and translational research, we will find ways to help them get better.”
Question of the Year:
What was the most significant challenge in your field in 2020?
The challenge for our field in 2020 has been the evolution of in-person management of complex diseases such as diabetes to remote management—the need to change our practice to remain effective in helping our patients and retaining excellence in care.
- Zijian Chen, MD
Featured

Zijian Chen, MD
Assistant Professor of Medicine (Endocrinology, Diabetes, and Bone Disease); Medical Director, Center for Post-COVID Care