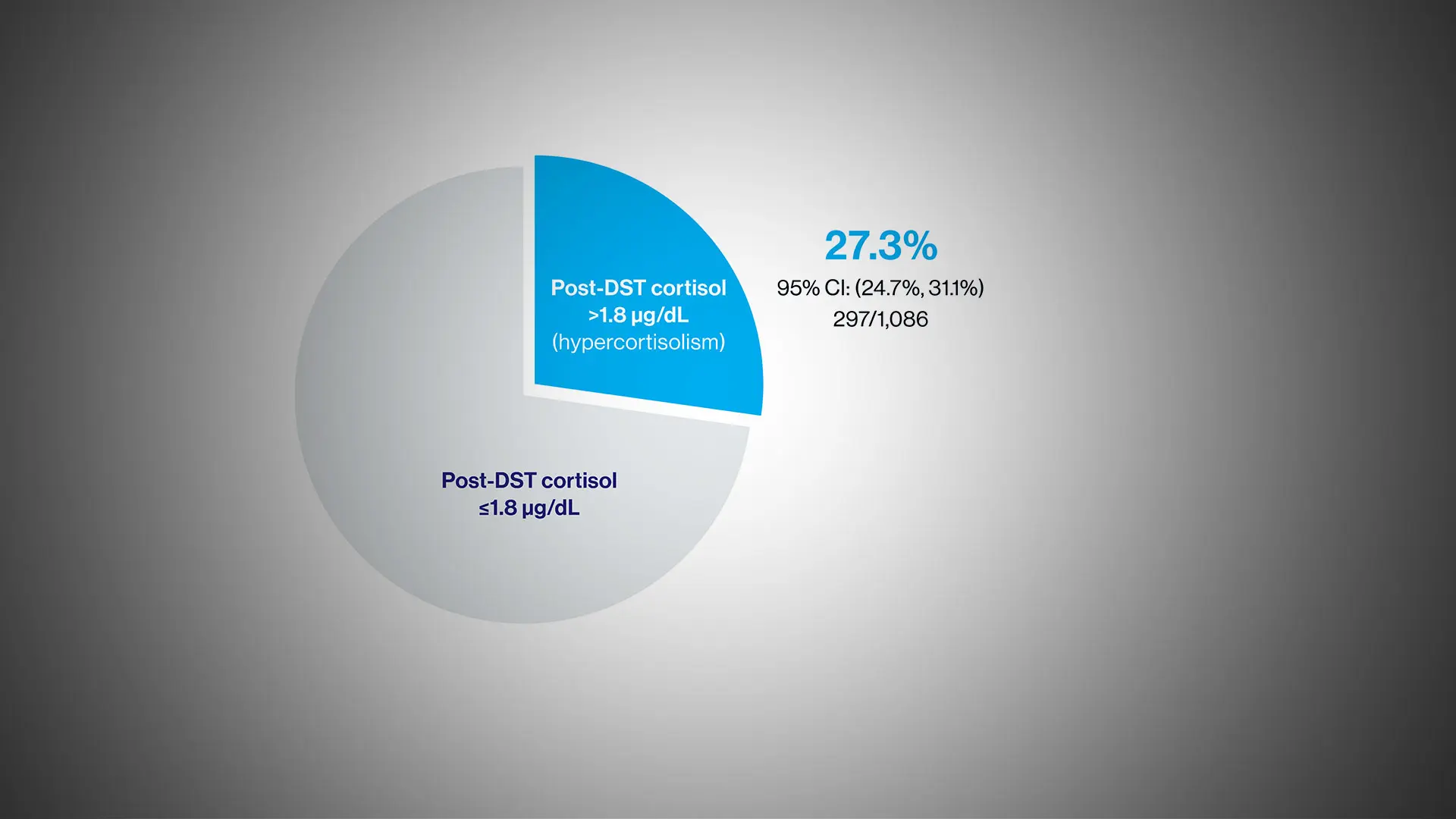
A multicenter observational study found that 27 percent of patients with resistant hypertension have hypercortisolism. “This finding demonstrates that hypercortisolism is more common in these patients than previously understood by researchers and physicians,” says principal investigator Deepak L. Bhatt, MD, MPH, MBA, Director of Mount Sinai Fuster Heart Hospital.
Resistant hypertension—where blood pressure remains high even though patients take three or more blood pressure medications—affects more than 10 million patients across the United States.
The study, known as MOMENTUM, is the first in the United States, and the largest, to investigate what percentage of patients with resistant hypertension have hypercortisolism. Dr. Bhatt presented the study as a featured clinical research presentation at the American College of Cardiology Scientific Session in March 2026.
“We are now beginning to understand that these patients may have other underlying medical conditions that make their blood pressure resistant to conventional treatments,” Dr. Bhatt says. “One of these conditions is hypercortisolism. Cortisol is commonly known as the ‘stress hormone,’ since it helps the body respond to stress, but cortisol itself becomes a serious problem if it’s high all the time.”
In the study, sponsored by Corcept Therapeutics Inc., researchers analyzed 1,086 patients at 50 centers across the United States, including the Mount Sinai Health System. Participants were adults age 18 and older with resistant hypertension, defined using the American Heart Association criteria (systolic blood pressure ≥130 mm Hg despite treatment with three or more antihypertensive medications of different classes at maximally tolerated doses, including a diuretic, or four or more medications from different classes regardless of systolic blood pressure). The participants were given a dexamethasone suppression test, which consisted of taking a tablet of dexamethasone before bedtime and getting a blood test to measure their cortisol level the next morning. If their cortisol level was greater than 1.8 ug/dL, they were considered to have hypercortisolism.
“The next step to further this research is conducting randomized trials to determine if therapies that lower the impact of cortisol can safely and effectively treat high blood pressure in these patients.”
Deepak L. Bhatt, MD, MPH, MBA
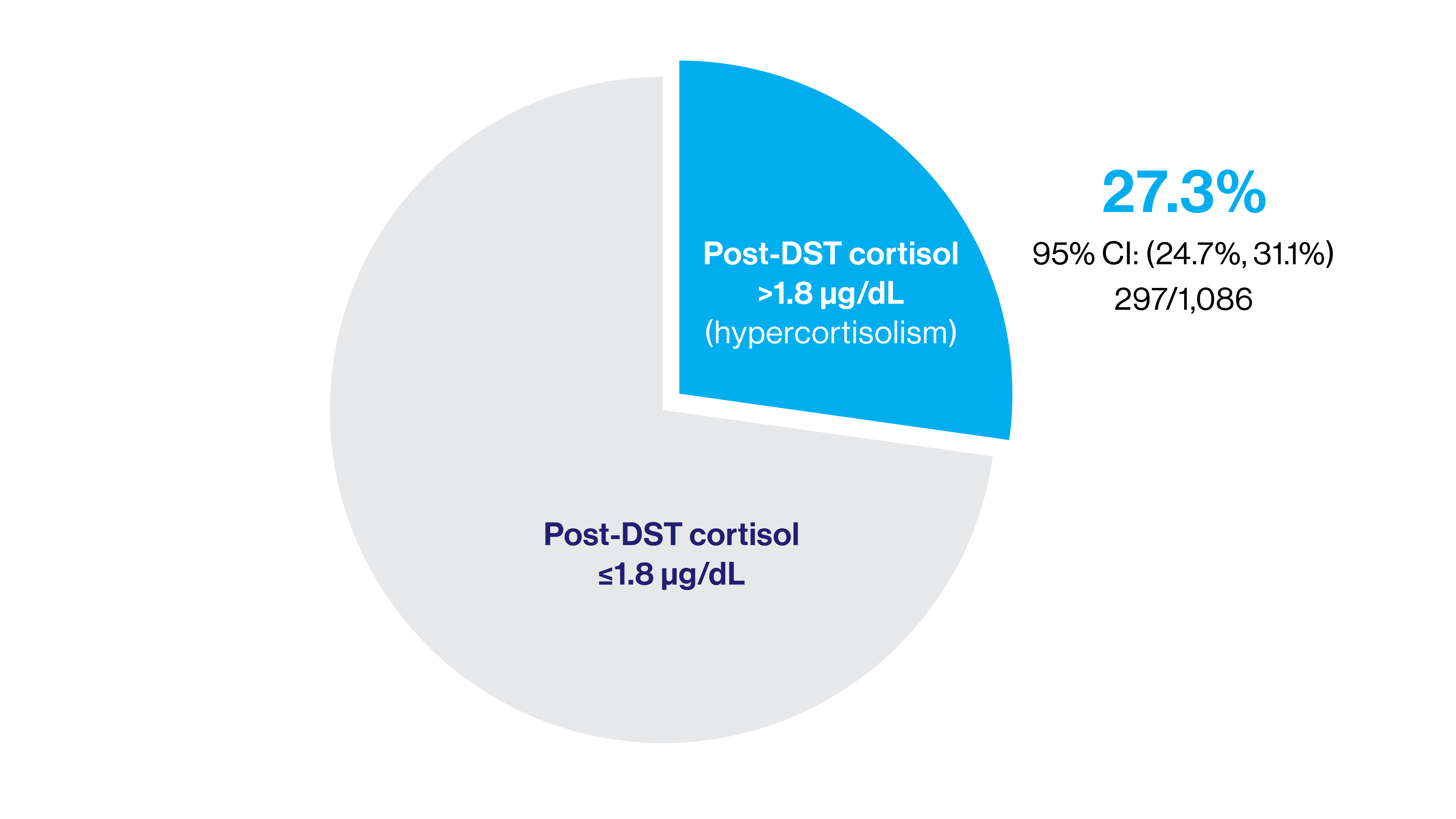
The prevalence of hypercortisolism in resistant hypertension patients from the MOMENTUM study.
The study found that 297 of the 1,086 participants, or 27 percent, had hypercortisolism. Researchers identified conditions, such as poor kidney function, that made it more likely for someone to have hypercortisolism. They also found that about 20 percent of participants had primary hyperaldosteronism, where the body makes too much of the hormone aldosterone, and about six percent of participants had both hypercortisolism and hyperaldosteronism.
Adults with resistant hypertension have an increased risk of ischemic heart disease, myocardial infarction, transient ischemic attack, stroke, end-stage renal disease, and premature mortality compared with those with controlled hypertension. Primary aldosteronism is a common—though widely underdiagnosed—cause of resistant hypertension, and endogenous hypercortisolism is another contributing cause that has been largely understudied, researchers say. The MOMENTUM findings point to options for physicians and patients.
“The fact that such a high percentage—more than 25 percent—of patients with resistant hypertension have elevated cortisol levels is very different from what doctors have been historically taught in medical school. These findings should prompt more screening for excess levels of cortisol in patients with resistant hypertension,” Dr. Bhatt says. “The next step to further this research is conducting randomized trials to determine if therapies that lower the impact of cortisol can safely and effectively treat high blood pressure in these patients.”
Dr. Bhatt is a paid consultant for Corcept Therapeutics Inc.
Featured

Deepak L. Bhatt, MD, MPH, MBA
Director of Mount Sinai Fuster Heart Hospital, and the Dr. Valentin Fuster Professor of Cardiovascular Medicine