The Mount Sinai Health System in 2025 expanded STEMIcathAID, a secure mobile platform for ST-segment elevation myocardial infarction (STEMI) activation, coordination, and transfers across the Health System. The platform was developed by a team led by Annapoorna S. Kini, MD, Director of the Samin K. Sharma Family Foundation Cardiac Catheterization Lab at The Mount Sinai Hospital, and included interventional cardiologists, Emergency Department physicians, nurses, and operational partners. It is designed to reduce avoidable delays that can occur when critical information and decisions are distributed across sequential calls, ad hoc messaging, and multiple handoffs.
“This is a unique platform that is making the standard of care of STEMI patients more predictable, efficient, and urgent,” says Dr. Kini, the Zena and Michael A. Wiener Professor of Medicine at the Icahn School of Medicine at Mount Sinai.
STEMI care is uniquely vulnerable to “system friction.” Even when clinicians act with urgency, delays can be introduced by late EKG transmission to the receiving interventionalist, uncertainty about activation ownership across sites, or the operational complexity of arranging transport while preparing a Cath Lab in parallel. STEMIcathAID is intended to serve as a HIPAA-compliant coordination layer that standardizes early communication, keeps essential context in one place, and supports rapid multidisciplinary action.
When a STEMI is suspected, clinicians can initiate a structured activation within the app and attach essential clinical details, including the EKG. Predefined roles are notified in parallel so downstream clinical and operational teams receive the same alert at the same time, reducing reliance on cascades of calls and repeat relays of the same information.
The platform’s key capabilities include:
Role-based notifications to reach emergency medicine, cardiology, interventional cardiology, Cath Lab staff, and transfer/operations teams quickly
EKG transmission and shared clinical context to support timely case confirmation and consistent decision-making
Secure team communication via chat and, when needed, video-based discussion
Operational visibility during transfers (including transport tracking where applicable) to help receiving teams align staffing and room readiness with expected arrival timing
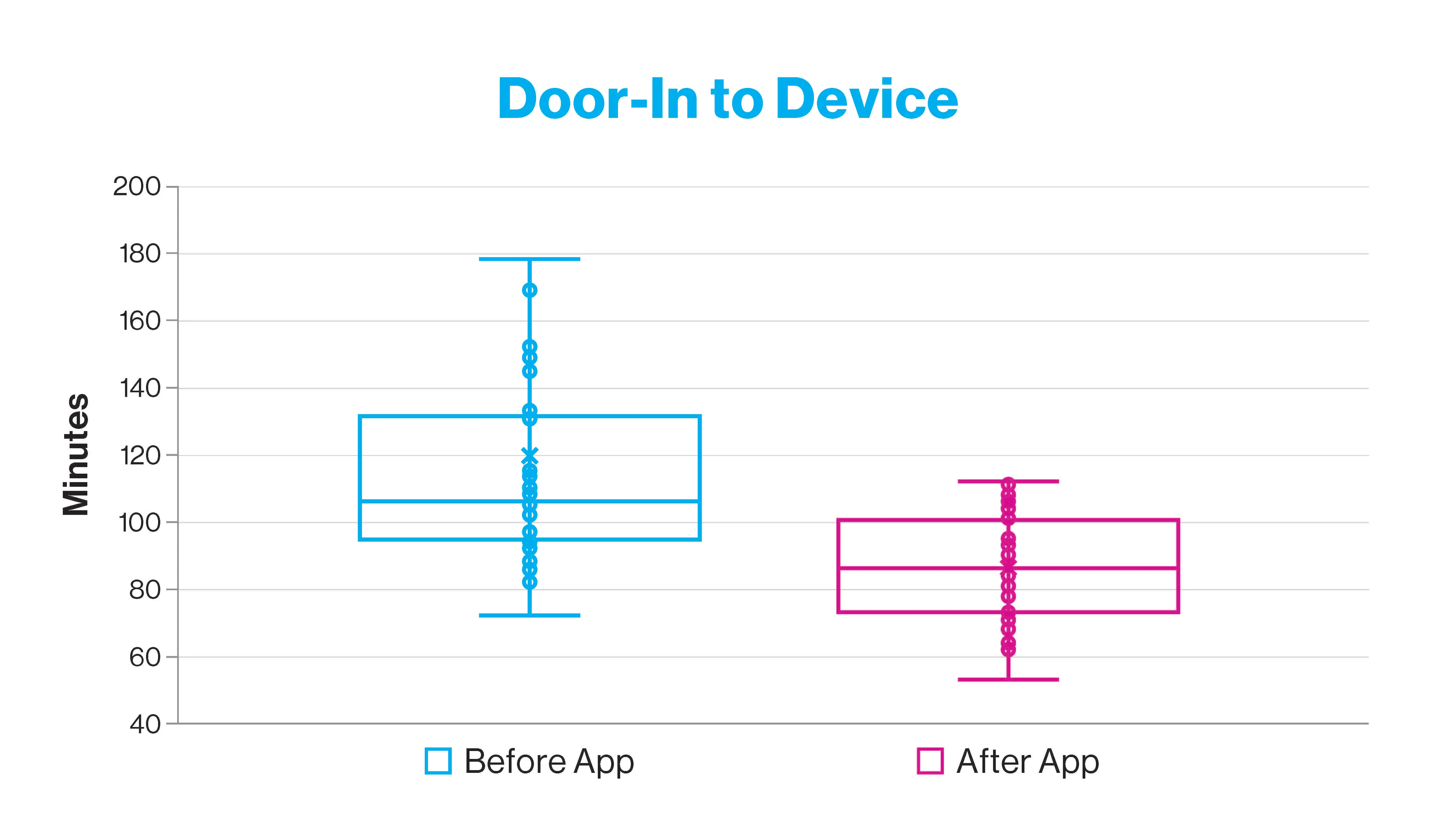
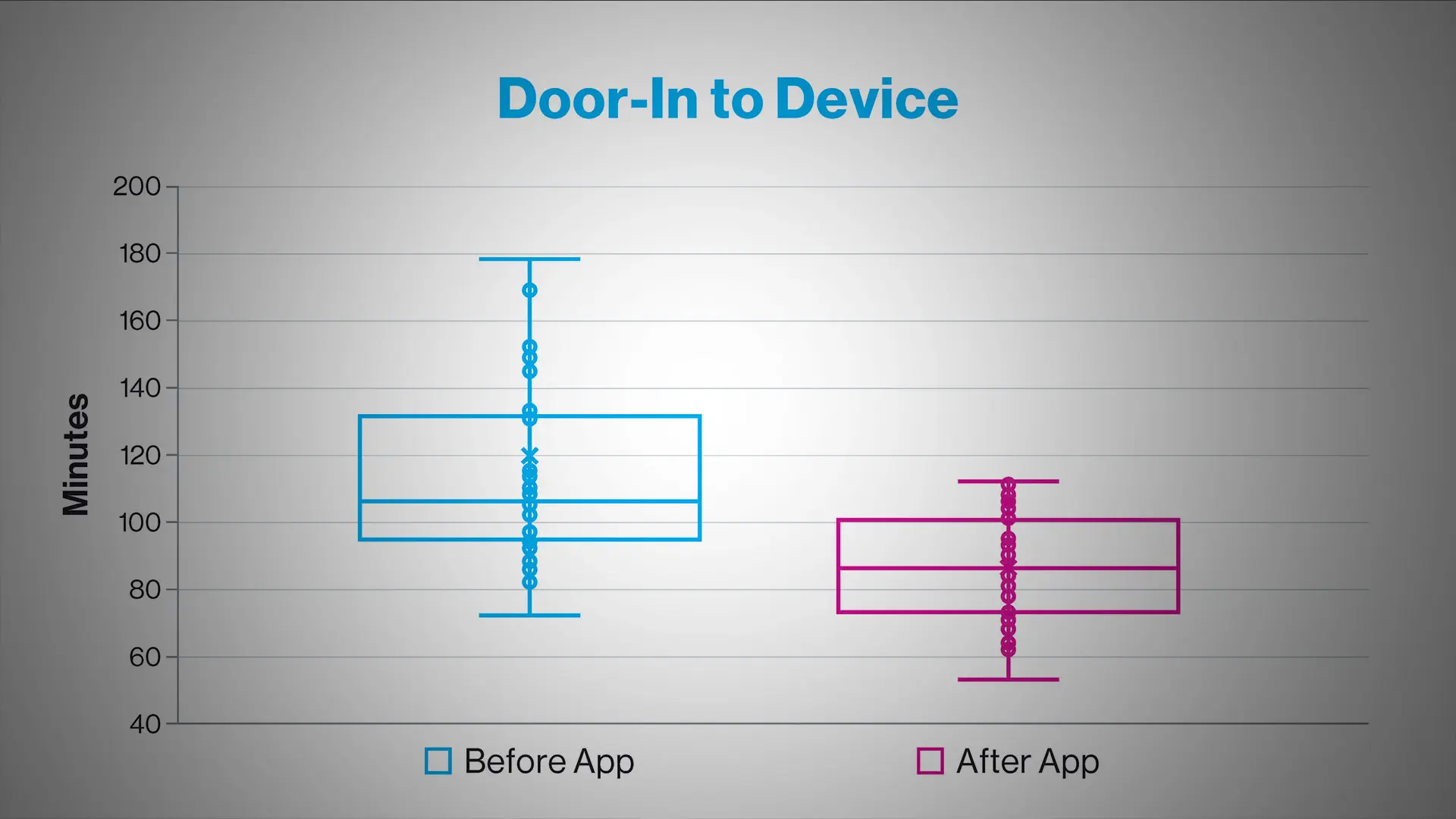
First ED door-to-device time for STEMI transfer patients before and after STEMIcathAID implementation.
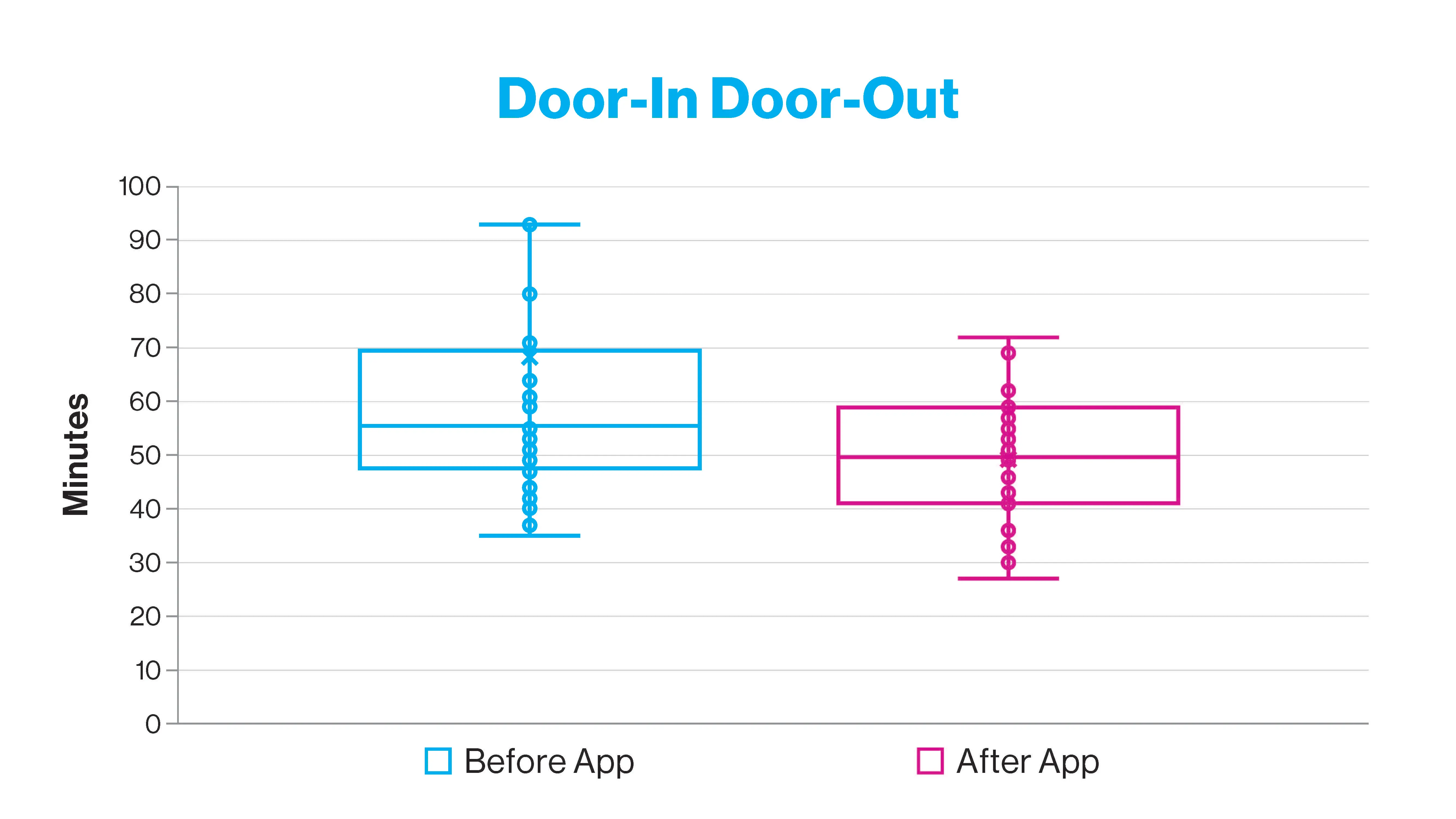
The effect of the app implementation on the door-in-door-out time at the STEMI referring hospital.
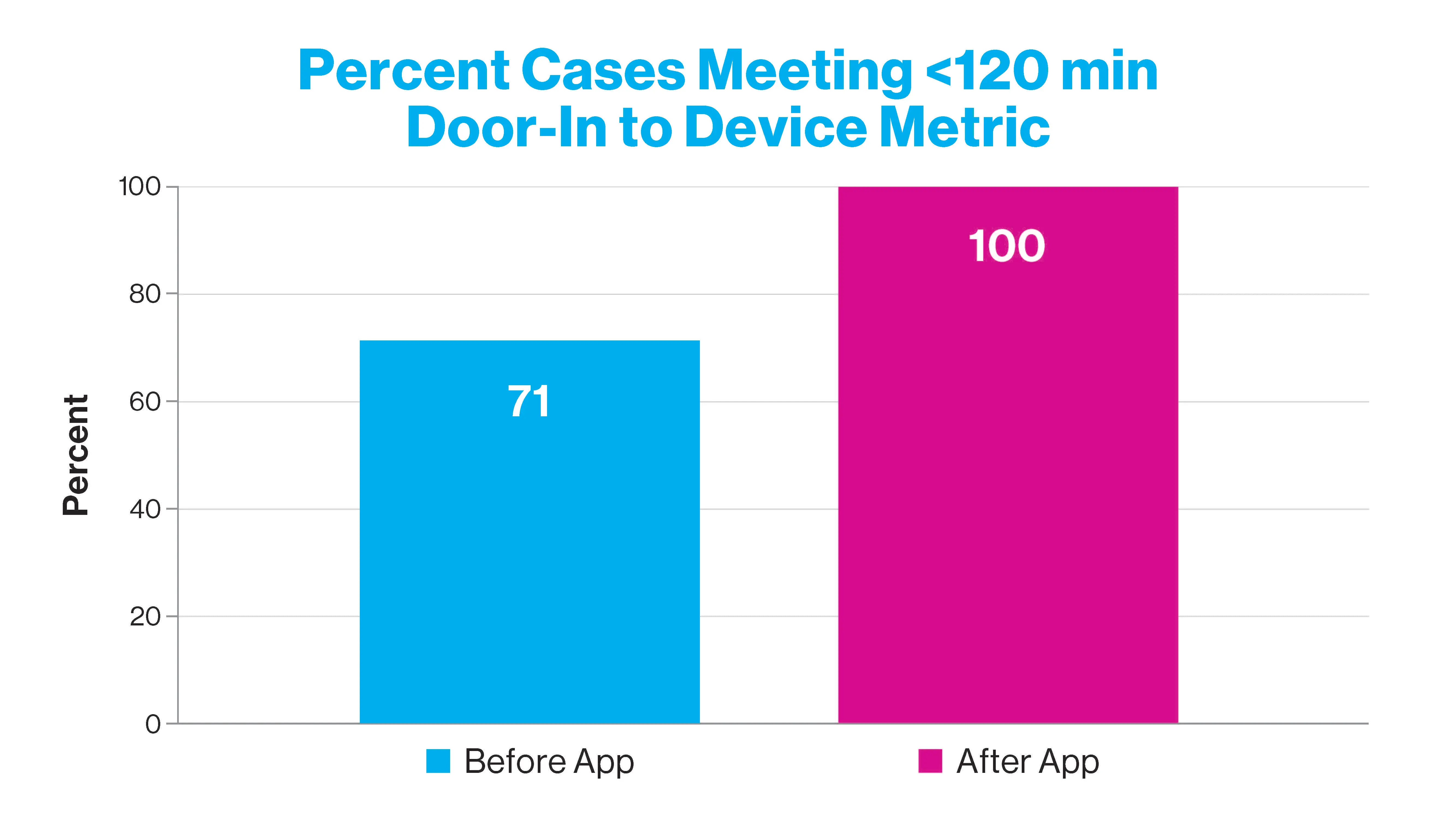
Percent of cases meeting AHA metric of 120 minutes for door-to-device time, before and after app.
Results of the Mount Sinai Hospital-Mount Sinai Queens pathway were published in 2024 in the International Journal of Cardiology, showing promising benefits.
The study found that from July 2021 to February 2023, 111 suspected STEMI calls were activated through the app, with 66 accepted and 45 rejected cases. In the study, 31 STEMI cases using the new platform were compared with 42 previous STEMIs that were activated through the traditional pathway before the app implementation. Median door-to-device time for STEMIcathAID-assisted transfer decreased from 106 minutes to 86 minutes. This significant improvement of the key metric for interhospital transfer resulted in all STEMI cases meeting the American Heart Association’s goal of door-to-device time of 120 minutes or less. In addition, median door-in-door-out time at the referral hospital decreased from 56 minutes to 50 minutes.
The expansion of the STEMI platform required more than adding users, the team says. Workflows differ meaningfully across hospitals—even within a single health system—such as staffing patterns, escalation practices, and facility logistics. Those differences influence where delays accumulate and which segments of the activation-to-reperfusion chain are most responsive to intervention.
Deployment followed a structured, multidisciplinary process spanning emergency medicine, cardiology, interventional cardiology, Cath Lab leadership, nursing leadership, transfer/operations teams, and the implementation team. Workgroups mapped current-state processes, defined a standardized “future-state” workflow inside the application, and refined notification logic so the initial alert reliably reached the appropriate on-site responder and supervising attending while also notifying the receiving interventional team, with downstream alerts to Cath Lab personnel after case acceptance.
As new pathways were added, the platform evolved to match local realities. Sites that incorporate residents in early STEMI evaluation required a resident role that can initiate an alarm under attending oversight. Local PCI-capable activations highlighted different operational dependencies, such as after-hours access and internal transport, supporting creation of operational roles (for example, security) so essential nonclinical partners could participate in time-critical coordination.
Role-specific training materials were adapted by site, access lists were finalized for ED and Cath Lab teams, onboarding was supported across available clinical devices (including Rover positioning devices where applicable), and full-scale simulations tested the end-to-end activation and transfer communication chain prior to go-live. Go-live proceeded only after alert delivery and workflow integrity were confirmed under realistic conditions.
Future priorities include standardized milestone definitions and more automated time capture, ideally through integration of electronic health records, to reduce missing data and enable segment-level analyses (e.g., activation-to-acceptance, acceptance-to-departure). Expansion to additional pathways and other time-sensitive disease states is being explored, and the team is working on a system-level analysis of the platform.
“By scaling STEMIcathAID across distinct transfer and local emergency workflows, Mount Sinai is advancing a repeatable approach to STEMI coordination,” Dr. Kini says. “This very effectively emphasizes rapid notification, shared clinical context, and operational visibility, supporting consistent delivery of guideline-directed reperfusion care across the Health System.”
For more information about the STEMI app and other cardiology applications designed to share knowledge with physicians around the world, go to Cardiology Apps.
Featured

Annapoorna S. Kini, MD
Director of the Cardiac Catheterization Laboratory at The Mount Sinai Hospital, and the Zena and Michael A. Wiener Professor of Medicine

Samin K. Sharma, MD
Director of Interventional Cardiology, The Mount Sinai Hospital, and Anandi Lal Sharma Professor of Medicine in Cardiology