Transcatheter mitral valve repair for heart failure patients with mitral regurgitation can reduce the long-term rate of hospitalizations by almost 50 percent, and death by nearly 30 percent, compared with heart failure patients who don’t undergo the procedure, according to a multicenter study led by Gregg W. Stone, MD, Director of Academic Affairs for the Mount Sinai Health System and Professor of Medicine (Cardiology), at the Icahn School of Medicine at Mount Sinai.
The trial is the largest to examine the safety and effectiveness of transcatheter mitral valve repair in a heart failure population using Abbott’s MitraClip™ system. It shows this treatment option significantly improves outcomes for patients with heart failure that do not respond to conventional treatments.
The five-year results from the Cardiovascular Outcomes Assessment of the MitraClip Percutaneous Device (COAPT) study were announced in March 2023 as a late-breaking clinical trial presentation at the American College of Cardiology Scientific Sessions Together with World Congress of Cardiology (ACC.23/WCC) in New Orleans, and published in The New England Journal of Medicine.
“Treating severe secondary mitral regurgitation in appropriate patients with cardiomyopathy is important—our study shows that five years after the MitraClip procedure, patients feel better, are hospitalized less frequently, and live longer,” says Dr. Stone. “It’s critical for physicians to recognize severe mitral regurgitation in patients with cardiomyopathy, then treat this secondary issue as early as possible to improve outcomes in this heart failure group.”
Roughly 30 percent of patients with left ventricular cardiomyopathy go on to develop severe secondary mitral valve regurgitation, in which the mitral valve becomes distorted from the enlarged left ventricle so its leaflets do not completely close. This regurgitation increases the pressure in the heart and puts patients at increased risk of hospitalization and death. In most patients, this condition can be treated with the minimally invasive procedure transcatheter edge-to-edge repair (TEER) in which the leaflets of the mitral valve are clipped together. The procedure is commonly performed with the MitraClip.
“Within five years, heart failure patients treated with MitraClip were on average alive and out of the hospital for 229 days more—eight full months—than patients treated with medications alone. ”
Gregg W. Stone, MD
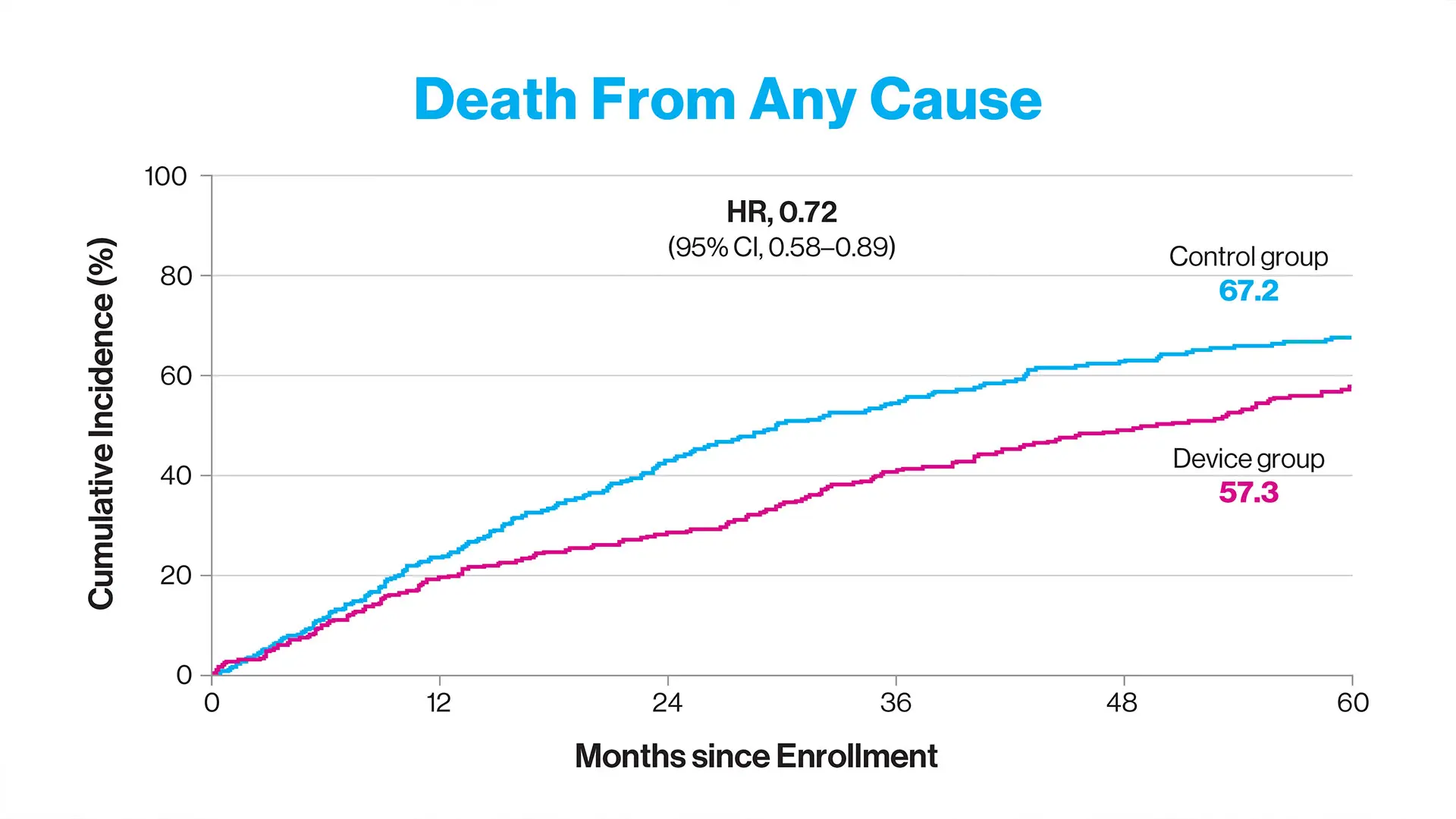
Transcatheter mitral valve repair for heart failure patients with mitral regurgitation can reduce death by nearly 30 percent, compared with heart failure patients who don’t undergo the procedure.
In the COAPT study, which was funded by Abbott, researchers investigated whether treating the severe secondary mitral valve regurgitation with TEER, which has no direct effect on the underlying weakened heart muscle, would improve overall outcomes in heart failure patients beyond medical therapy alone. The two-year results, published in 2018, showed for the first time that treating secondary mitral valve regurgitation improved patients’ symptoms, reduced hospitalizations, and led them to live longer. The latest five-year results show further significant findings.
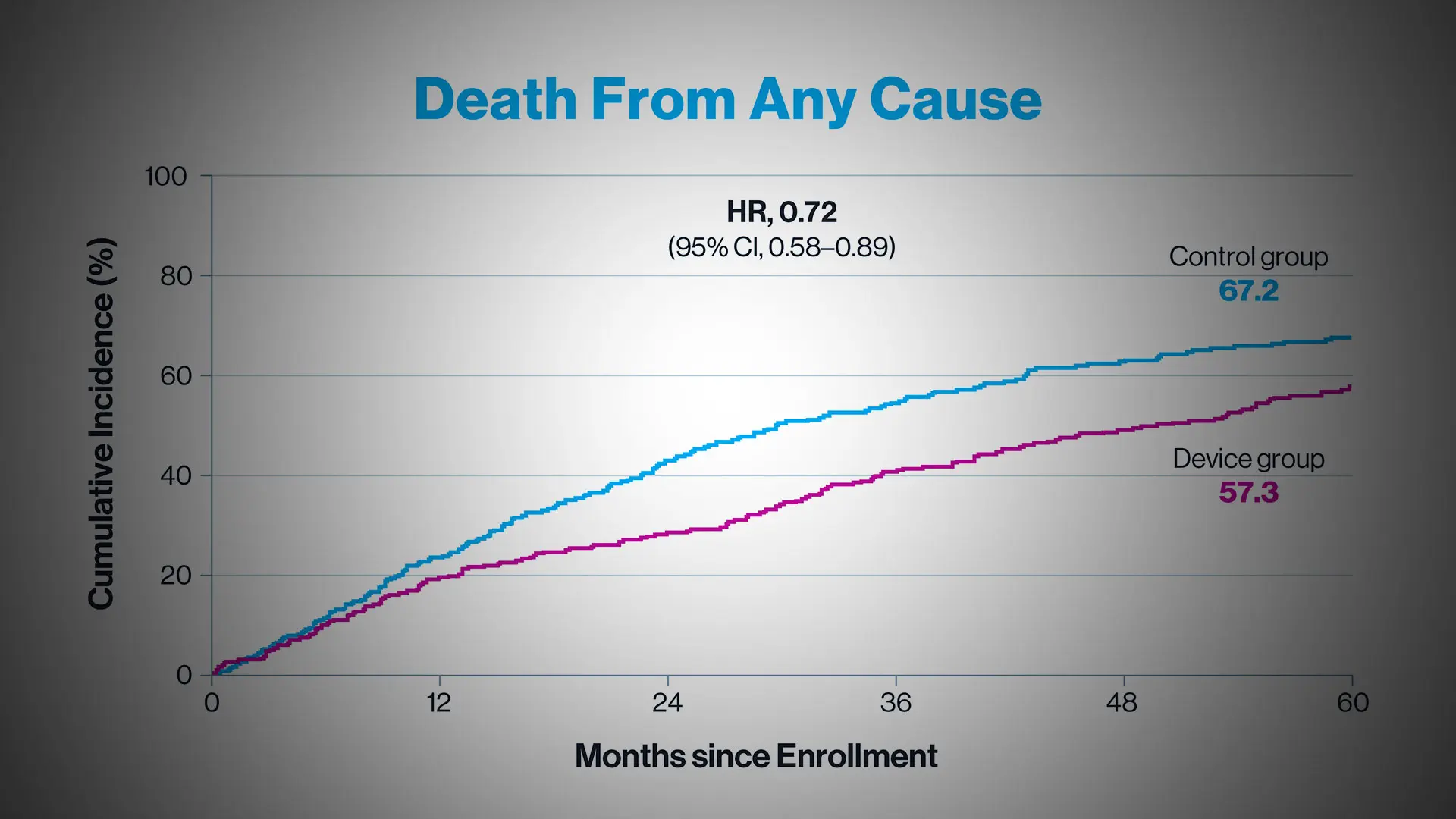
In the five-year follow-up study, researchers analyzed 614 patients enrolled between December 27, 2012, and June 23, 2017, at 78 sites in the United States and Canada. All patients had cardiomyopathy and secondary, severe mitral valve regurgitation despite treatment with optimal medical therapy for heart failure. Half of those patients continued their heart failure medication, while the other half underwent transcatheter valve repair with the MitraClip while continuing on the heart failure medication. Over the five years following treatment, the yearly rates of heart failure hospitalizations were 33.1 percent in the MitraClip group compared to 57.2 percent with patients treated with medications only, which was a 47 percent reduction. Deaths from heart failure were reduced by 29 percent in the MitraClip group compared with patients treated with medications only, and all-cause death was reduced by 28 percent.
Even though patients in the MitraClip group had fewer deaths and hospitalizations after successful treatment, at the end of five years, 73.6 percent of them died or had one or more heart failure hospitalizations (compared to 91.5 percent of patients in the medication-only group). Dr. Stone says this result highlights the need for advanced therapies to treat these high-risk patients.
“Within five years, heart failure patients treated with MitraClip were on average alive and out of the hospital for 229 days more—eight full months—than patients treated with medications alone. Thus, MitraClip treatment provided great benefits for these patients in terms of longevity and quality of life,” says Dr. Stone. “However, the TEER procedure doesn’t cure the underlying damaged heart muscle, and the long-term prognosis of these patients is worse than for many cancers. New medical therapies and device-based treatments for heart failure that can lower the pressures and blood volume within the heart or take over its pumping function are essential to further improve the quality of life and longevity in these desperate patients.”
Dr. Stone has served as a consultant to Abbott, and The Mount Sinai Hospital receives research grants from Abbott. Dr. Stone also works with other companies that are developing devices to reduce mitral regurgitation.
Featured

Gregg W. Stone, MD
Professor of Medicine (Cardiology), and Population Health Science and Policy